A torn anterior cruciate ligament changes a knee in very specific ways, and a well-executed reconstruction changes it back in equally specific ways. Patients considering surgery want to know what actually shifts between the “before” and the “after,” measured not in feelings alone but in pain scores, strength numbers, hop distances, stability exam grades, and how often people get back to the sports they loved. The published evidence, including data generated by the surgical team at Ochsner-Andrews Sports Medicine Institute, gives a clear answer to each of those questions. This page translates that evidence into plain language, dimension by dimension, so patients in Baton Rouge and beyond can set expectations grounded in outcomes data rather than anecdote.
📋 In This Article
- Before: What a Torn ACL Actually Looks Like
- Surgery: The Inflection Point
- After: Patient-Reported Outcomes at 1 and 2 Years
- Function and Strength: What “Cleared” Does and Doesn’t Mean
- Activity Level: Return to Sport vs. Return to Pre-Injury
- Symptom Trajectory: Pain, Swelling, Stability Over Time
- Re-Tear Risk and Long-Term Outlook
- Frequently Asked Questions
Before: What a Torn ACL Actually Looks Like
The injury moment is usually unmistakable. Roughly 70% of ACL tears happen in non-contact situations (a cut, a pivot, a landing), and patients typically describe an audible “pop,” rapid swelling within a few hours, and a sense that the knee buckled or “came apart.” On examination in the days that follow, a deficient ACL produces a positive Lachman test (excessive anterior tibial translation relative to the femur) and, with the patient relaxed or under anesthesia, a positive pivot shift (a palpable and often visible reduction of the tibia as the knee moves through 20 to 30 degrees of flexion). Both tests, when performed by an experienced examiner, are highly specific for a torn ACL.
Imaging confirms what the exam suggests. MRI shows discontinuity or nonvisualization of the ACL fibers, typical bone bruise patterns in the lateral femoral condyle and posterolateral tibial plateau, and (in many cases) concomitant meniscal injury. The published PIVOT cohort, in which Dr. Burnham was a study group investigator, demonstrated that concurrent meniscal pathology is present in a substantial share of ACL-injured knees: 38% of the cohort had medial meniscal lesions treated at the time of reconstruction, and 28% had lateral meniscal lesions (Diermeier et al., 2020).
The functional picture before surgery is consistent. Patient-reported IKDC subjective scores in the PIVOT cohort averaged 56.5 points out of 100 preoperatively, and activity-of-daily-living scores averaged 75.7 out of 100. Patients at this baseline are typically limiting stairs, avoiding cutting sports, and experiencing episodes of giving way that erode their confidence in the knee.
Surgery: The Inflection Point
Anatomic ACL reconstruction is the structural intervention that restores the restraint the native ligament used to provide. Using an inertial sensor and tablet-based image analysis during intraoperative pivot shift testing, the PIVOT study quantified the change in real time. Side-to-side anterior tibial translation fell from a preoperative average of 2.0 mm to −0.1 mm immediately after reconstruction, and side-to-side tibial acceleration fell from 2.6 m/s² to −0.5 m/s² . In other words, the reconstructed knee was indistinguishable from the uninjured contralateral knee on the operating table, with the patient still under anesthesia (Diermeier et al., 2020).
Restoring that passive restraint is necessary but not sufficient. The restoration of rotational stability at time zero does not, by itself, guarantee the patient will perform well one or two years later; that outcome depends heavily on graft choice, surgical technique, individualized indications for additional procedures such as lateral extra-articular tenodesis, and the quality of the rehabilitation that follows (Giusto et al., 2025). For most primary reconstructions in active adults and athletes, however, the operation reliably returns the knee’s mechanical starting point to near-normal. Understanding the criteria for choosing the right ACL surgeon is essential to ensuring optimal surgical outcomes.
After: Patient-Reported Outcomes at 1 and 2 Years
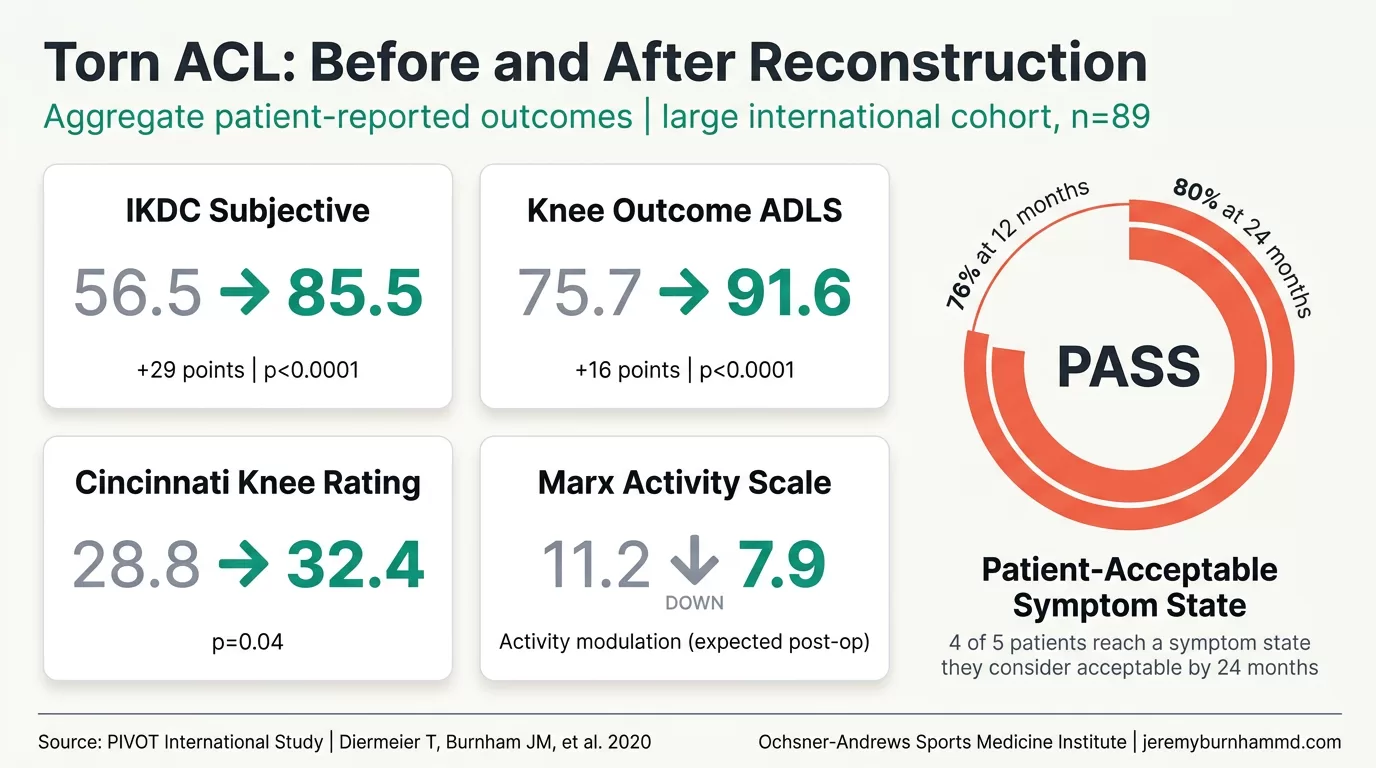
Patient-reported outcomes (PROs) are the gold standard for measuring how much better a patient actually feels and functions. The PIVOT cohort followed 89 patients for two years after anatomic ACL reconstruction with hamstring autograft and reported the following trajectory (Diermeier et al., 2020):
- IKDC subjective knee score (0 to 100; higher is better): 56.5 preoperatively, 84.5 at 12 months, 85.5 at 24 months. A 29-point improvement is well beyond the minimal clinically important threshold.
- Activity of Daily Living Score (0 to 100): 75.7 preoperatively, 92.2 at 12 months, 91.6 at 24 months.
- Cincinnati Knee Rating System: 28.8 preoperatively, 32.4 at 24 months.
- Marx activity rating: 11.2 preoperatively, 7.9 at 24 months, reflecting the expected modulation of high-impact activity after injury.
An equally important endpoint is whether a patient has reached what researchers call the Patient Acceptable Symptom State (PASS), defined for the IKDC as a score of 75.9 or higher. In the PIVOT cohort, 76% of patients had reached PASS at one year and 80% by two years. The clinical translation is straightforward: four out of five patients, at two years from a well-performed anatomic reconstruction, rate their knee as acceptably symptom-free for the demands of their life.
Function and Strength: What “Cleared” Does and Doesn’t Mean

Symptom scores capture part of the picture. Objective strength and hop testing capture the rest, and they frequently tell a more sobering story than the patient’s self-report. In a prospective study by Kline, Burnham, and colleagues, patients who had been cleared for return to play after ACL reconstruction were tested against the contralateral uninjured limb. The reconstructed limb still lagged meaningfully on every metric (Kline et al., 2017):
- Single-leg hop distance: 146 ± 37% of limb length on the operated side vs. 182 ± 38% on the contralateral side.
- Triple hop distance: 417 ± 106% vs. 519 ± 102%.
- Crossover hop distance: 364 ± 107% vs. 446 ± 123%.
- Timed 6-meter hop: 3.3 ± 2.0 seconds vs. 2.3 ± 0.6 seconds.
- Knee extension strength: 308 ± 120 N vs. 366 ± 119 N.
The quadriceps deficit after ACL reconstruction is not a training error; it is a predictable neurophysiologic phenomenon called arthrogenic muscle inhibition (AMI). The injury and subsequent surgery alter the reflex drive from joint mechanoreceptors to the quadriceps motor pool, which voluntarily quiets down even when the muscle is structurally intact (Konishi et al., 2002). The implication is that a rehabilitation program aimed at restoring quadriceps strength has to start neurologically, with deliberate activation drills within the first few postoperative days, before it can progress to the eccentric and functional loading that builds true symmetry over months. Published frameworks from Diermeier and colleagues describe this neural re-engagement approach in detail (Diermeier et al., 2020).
Clinical Translation
Being “cleared for sport” is a checkpoint, not a finish line. Published data show that a meaningful minority of patients with apparently normal PROs still carry quad and hop deficits of 15% or more at the time of clearance. That gap is the single biggest driver of second ACL injury risk in the first year back.
Activity Level: Return to Sport vs. Return to Pre-Injury
Return-to-sport statistics are easy to misinterpret because “sport” can mean recreational jogging or NCAA Division I competition. The published literature separates these tiers cleanly. A landmark meta-analysis pooling 48 studies and more than 5,700 patients reported that 81% of patients returned to any level of sport, 65% returned to their preinjury level of sport, and 55% returned to competitive sport after reconstruction (Ardern et al., 2014). Within anatomic single-bundle reconstruction specifically, reported rates are higher in recent cohorts, with 92% return to sport at a minimum of two years from surgery reported by Kowalczuk and Burnham (2017).
The timing of return is as important as the eventual rate. Grindem and colleagues demonstrated that every one-month delay in return to sport beyond the six-month mark reduced the rate of reinjury by 51%, up to the nine-month threshold, and that passing a battery of objective return-to-sport criteria independently cut reinjury risk by two-thirds (Grindem et al., 2016). The Ochsner-Andrews Sports Medicine Institute ACL Center of Excellence rehabilitation protocol uses that evidence base, pairing time (typically a minimum of nine months from surgery) with criterion-based milestones (quad LSI ≥ 90%, hamstring LSI ≥ 90%, full hop battery LSI ≥ 90%, successful plyometric progression, and sport-specific drill clearance).

Patient story: Alexis Rodriguez tore her ACL on a fast-break layup and returned to basketball after reconstruction at Ochsner-Andrews Sports Medicine Institute.
Symptom Trajectory: Pain, Swelling, Stability Over Time
Symptoms do not improve linearly, and patients who understand the rhythm tolerate the process better. The following milestones reflect published evidence-based rehabilitation frameworks (van Melick et al., 2016) and the team’s clinical experience at the Ochsner-Andrews ACL Center of Excellence.
- Weeks 1 to 2: Incisional pain, moderate effusion, quadriceps shutdown. Range of motion is the priority. For isolated reconstructions, weight-bearing as tolerated with a brace locked in extension for ambulation. Concurrent meniscal repair modifies this timeline.
- Weeks 3 to 6: Swelling declines; full extension is established; flexion approaches 120 degrees. Pain becomes activity-related rather than constant. Neuromuscular quadriceps drills intensify.
- Month 3: Most patients walk without a limp; stairs are negotiated reciprocally. Strength training progresses to moderate resistance. Running is not yet permitted.
- Month 6: Running progression begins if quad strength reaches approximately 70% of the contralateral limb. Plyometric progression starts. The knee feels increasingly “like mine,” but asymmetry on hop testing is still typical.
- Month 9: Criterion-based testing occurs. Quad and hamstring LSI targets are 85% to 90%; hop battery LSI target is 90%. Patients who pass begin sport-specific drill progression.
- Month 12: Unrestricted return to sport for patients who have met all criteria. Retesting occurs throughout the first year back.
Patients commonly report that the knee feels “different but normal” somewhere in the six-to-nine-month window, and that the last 10 to 15% of confidence returns only with repeated successful exposure to sport-specific load. That psychological component is real and is tracked in clinic with validated tools such as the ACL-RSI scale.
Re-Tear Risk and Long-Term Outlook
A small but real percentage of reconstructions fail. In the PIVOT two-year data, traumatic graft retear occurred in 4.5% of patients (4 of 89), all from significant new injuries (Diermeier et al., 2020). Kowalczuk and Burnham reported a 5% retear rate at minimum two-year follow-up in anatomic single-bundle reconstructions. Across larger registries, the range is typically 3% to 10%, with the highest rates in young female athletes returning to cutting and pivoting sport before criterion-based milestones are met.
Longer-term, the issue that matters most is cartilage preservation. Residual rotational laxity at one to two years, even when the patient is asymptomatic, correlates with later radiographic osteoarthritis at five to nine years (Jonsson et al., 2004). That correlation is the clinical reason to aim for complete rotational restoration at the index surgery, with appropriate attention to meniscal preservation and, in select cases, lateral extra-articular augmentation (Giusto et al., 2025).
About Dr. Jeremy Burnham
Dr. Jeremy Burnham is a board-certified orthopaedic surgeon at Ochsner-Andrews Sports Medicine Institute in Baton Rouge and the most published ACL surgeon in Louisiana. His clinical practice focuses on complex knee ligament reconstruction, primary and revision ACL surgery, meniscus repair, and cartilage preservation, with an emphasis on returning athletes to sport after injury. At Ochsner Health he serves as System Vice Chair of the Musculoskeletal Service Line and Regional Department Head of Orthopedic Surgery & Sports Medicine. His research has produced 53 peer-reviewed publications and 13 book chapters, several of which are cited on this page, and he is site principal investigator on the NIH- and DoD-funded STABILITY 2 trial (NCT03543098) and a member of the PIVOT International Study Group. He is a recipient of the Louisiana Arthritis Foundation Game Changer Award (2025) and the AOSSM Playmaker Grant (2022). Residency at the University of Kentucky under Drs. Darren Johnson, Mary Lloyd Ireland, and Christian Lattermann; fellowship at the University of Pittsburgh (UPMC) under Drs. Freddie Fu, James Bradley, and Volker Musahl.
References
- Diermeier T, Meredith SJ, Irrgang JJ, et al. Patient-Reported and Quantitative Outcomes of Anatomic ACL Reconstruction With Hamstring Tendon Autografts. Orthop J Sports Med. 2020;8(7):2325967120926159. DOI · PubMed · JMB PDF
- Kline PW, Burnham J, Yonz C, Johnson DL, Ireland ML, Noehren B. Hip external rotation strength predicts hop performance after anterior cruciate ligament reconstruction. Knee Surg Sports Traumatol Arthrosc. 2018;26(4):1137-1144. DOI · PubMed · JMB PDF
- Burnham JM, Drazick AI, Aminake G, et al. Current Concepts in Hip and Core Assessment to Reduce the Risk of ACL Injury. Int J Sports Phys Ther. 2026. DOI · PubMed · JMB PDF
- Giusto JD, Burnham JM, Dadoo S, et al. Lateral extra-articular tenodesis augmentation of primary ACL reconstruction: indications and outcomes. J ISAKOS. 2025. DOI · PubMed
- Ardern CL, Taylor NF, Feller JA, Webster KE. Fifty-five per cent return to competitive sport following anterior cruciate ligament reconstruction surgery: an updated systematic review and meta-analysis including aspects of physical functioning and contextual factors. Br J Sports Med. 2014;48(21):1543-1552. DOI · PubMed
- Grindem H, Snyder-Mackler L, Moksnes H, Engebretsen L, Risberg MA. Simple decision rules can reduce reinjury risk by 84% after ACL reconstruction: the Delaware-Oslo ACL cohort study. Br J Sports Med. 2016;50(13):804-808. DOI · PubMed
- van Melick N, van Cingel REH, Brooijmans F, et al. Evidence-based clinical practice update: practice guidelines for anterior cruciate ligament rehabilitation based on a systematic review and multidisciplinary consensus. Br J Sports Med. 2016;50(24):1506-1515. DOI · PubMed
- Kowalczuk M, Burnham JM, Uquillas C, et al. Individualized anatomic anterior cruciate ligament reconstruction. ACL Masters: Advanced Concepts in ACL Management. Springer; 2017.
- Konishi Y, Fukubayashi T, Takeshita D. Possible mechanism of quadriceps femoris weakness in patients with ruptured anterior cruciate ligament. Med Sci Sports Exerc. 2002;34(9):1414-1418. DOI · PubMed
- Jonsson H, Riklund-Ahlstrom K, Lind J. Positive pivot shift after ACL reconstruction predicts later osteoarthrosis: 63 patients followed 5-9 years after surgery. Acta Orthop Scand. 2004;75(5):594-599. DOI · PubMed
Frequently Asked Questions
What is the first thing that changes after ACL surgery?
Mechanical stability changes first. Intraoperative measurements during the PIVOT study showed that anatomic reconstruction restored side-to-side anterior tibial translation from roughly 2 mm of excess laxity preoperatively to near zero immediately after graft fixation. Patients typically feel a different, more stable knee from the first postoperative exam, although swelling and quadriceps shutdown mask that stability for the first several weeks.
When will my knee feel normal again?
Most patients describe the knee as different but normal somewhere between six and nine months postoperatively, with the last 10 to 15 percent of confidence returning during the first year back in sport. Patient-reported outcome scores rise most sharply in the first six months and plateau between 12 and 24 months, with 80 percent of patients reaching the Patient Acceptable Symptom State at two years.
Will I be able to play sports again after ACL surgery?
The published literature reports 81 percent return to any sport, 65 percent return to preinjury level, and 55 percent return to competitive sport after ACL reconstruction. Anatomic single-bundle reconstructions in active cohorts have reported return-to-sport rates as high as 92 percent at minimum two-year follow-up. Return is more likely when criterion-based milestones (quadriceps and hop limb symmetry greater than 90 percent) are met before release.
What is different about how my knee feels long-term?
Structural stability is typically excellent at two years, with published retear rates of roughly 4 to 5 percent in well-performed anatomic reconstructions. Most long-term differences are subtle: a small percentage of patients notice occasional stiffness, mild weather-related aching, or reduced kneeling tolerance. Cartilage preservation is the dominant long-term priority, and residual rotational laxity at one to two years is the strongest predictor of later osteoarthritis.
How do I know I am actually ready to return to sport?
Readiness is defined by evidence-based criteria rather than a calendar date. Published guidance supports a minimum of nine months from surgery combined with a quadriceps limb symmetry index of 90 percent or higher, a full hop battery symmetry index of 90 percent or higher, successful plyometric and sport-specific drill progressions, and a validated psychological readiness score. Patients who meet these criteria have reinjury rates that are meaningfully lower than patients released on time alone.
