Every credible orthopedic expert opinion begins with the medical record. Before any deposition, before any opinion letter, before any standard-of-care analysis, the expert sits down with the chart and reads it. Carefully. Page by page. Image by image. Visit by visit. The quality of the eventual opinion is a direct function of the thoroughness of that review, and a superficial pass through summaries and discharge notes will produce opinions that do not survive cross-examination.
Through Burnham Orthopedics & Sports Medicine, Dr. Jeremy Burnham provides systematic medical records review services for attorneys, adjusters, and parties evaluating orthopedic injury claims. The approach is grounded in a full-time clinical practice and a publication record of more than 145 peer-reviewed papers, book chapters, and scientific presentations spanning the diagnostic and treatment literature most relevant to musculoskeletal litigation, plus active site Principal Investigator roles on two federally funded ACL reconstruction trials (NIH STABILITY 2 and the Department of Defense STaR Trial). For attorneys, that translates into a records reviewer who reads the imaging the same way the operating surgeon does, knows what the published evidence actually says about each diagnostic modality, and can explain in plain language what the chart supports and what it does not. This page outlines what a systematic medical records review covers, the methodology that produces defensible opinions, and what attorneys should expect when retaining records review through Burnham Orthopedics & Sports Medicine. For related medicolegal services, see the orthopedic expert witness and independent medical examination pages. This review approach applies directly to workers’ compensation records review in Louisiana, where statutory timelines, physician selection rules, and benefit-type analysis depend on careful chart documentation across the six states served.
📋 In This Article
- What Medical Records Review Is (and Isn’t)
- When Attorneys Need a Records Review
- The Detective Work: What a Systematic Review Uncovers
- What’s in the Chart: Categories of Records
- Reading the Imaging: Knowing the Modality Limits
- Imaging Sensitivity for Specific Lesions
- The Imaging-Symptoms Gap
- Timeline Reconstruction and Causation Chains
- Pre-Existing vs. Acute Pathology
- Standard of Care vs. Outcome
- Documentation Standards
- The Records Review Deliverable
- What Attorneys Should Expect
- The Bottom Line
- Authoritative External Resources
- References
- Frequently Asked Questions
What Medical Records Review Is (and Isn’t)
A medical records review is a structured analytical exercise in which a qualified physician reads the complete clinical record of a patient or claimant and produces an opinion responsive to specific medical questions. In an orthopedic context, those questions typically concern causation (did the workplace event, motor vehicle accident, or alleged negligent act cause the condition for which the patient is now being treated), the appropriateness of the treatment provided, the existence and severity of permanent impairment, and the relationship between the imaging findings, the clinical examination, and the symptoms the patient reports. The reviewer is not the treating physician and is not assuming care of the patient. The American Academy of Orthopaedic Surgeons (AAOS) framework for medicolegal work is explicit on this point: the IME and records review physician “does not assume care of the patient” (Daniels et al., 2017).
What records review is not is also worth stating clearly. It is not advocacy. It is not a process designed to support a predetermined conclusion. The reviewer’s obligation is to the methodology, not to the retaining party. An expert who reads the same record for plaintiff and for defense should arrive at the same opinion both times, because the conclusions flow from the clinical data and the published literature, not from the identity of the client. When the chart supports the retaining party’s position, the review documents that. When the chart undermines the retaining party’s position, the review documents that too. Attorneys who understand this asymmetry get more value from the engagement than attorneys who treat the reviewer as an extension of the case theory.
Records review also is not the same as an independent medical examination. An IME involves a physical examination of the patient and is governed by state-specific procedural rules in workers’ compensation and insurance contexts; see the dedicated IME for Workers’ Compensation page for those frameworks. A records review is purely a paper-and-imaging exercise that may be conducted with or without an IME. Many engagements begin with records review alone and only proceed to an IME if the chart raises questions that cannot be resolved without examining the patient. The two services are complementary, not redundant.
When Attorneys Need a Records Review
The most common driver for retaining a records reviewer is a complex orthopedic injury claim in which the medical questions exceed what the case-handling attorney or adjuster can confidently evaluate from the file alone. In workers’ compensation, that often means causation disputes (did this event cause this injury, or did it aggravate a pre-existing condition that was destined to become symptomatic regardless), maximum medical improvement and impairment-rating disputes, treatment necessity disputes, and apportionment between covered and non-covered conditions. In personal injury litigation, records review supports motor vehicle accident cases involving alleged disc and joint injuries, premises liability cases involving slip-and-fall fractures and ligamentous injuries, and product liability cases involving orthopedic devices. In medical malpractice cases, records review is often the first step in standard-of-care analysis for surgical complications, missed diagnoses, and post-operative management.
Disability determinations and insurance coverage disputes also routinely benefit from records review. For long-term disability and Social Security determinations, the question is whether the documented impairment supports the functional limitations claimed. For coverage disputes, the question is whether the proposed treatment is medically necessary and appropriate given the documented diagnosis and prior treatment course. The economic stakes in these contexts are substantial; for context on the broader workers’ compensation environment, approximately 8.6 million nonfatal workplace injuries and 5,600 fatal injuries occur each year in the United States, with direct medical costs exceeding $67 billion and indirect costs exceeding $183 billion (Daniels et al., 2017). When the file is large, the medical history is layered, or the diagnosis is contested, an organized records review converts an unstructured stack of records into a defensible chronology of what happened, when, and what the evidence supports about why.
The Detective Work: What a Systematic Review Uncovers
The most useful framing for what a records review actually does is investigative. The reviewer is looking for the objective findings that the chart documents, the timeline of those findings, the consistency of the clinical picture across providers, and the gaps or contradictions that the routine clinical workflow may not have flagged. Most charts contain more information than any single treating physician had time to integrate. A treating orthopedist may have made decisions based on the visit in front of them, without revisiting prior MRI characteristics or comparing today’s exam to the physical therapy notes from six months earlier. A pain management physician may have escalated medications without correlating to whether the imaging actually changed. The records reviewer’s job is to integrate all of it.
The yield of that work is often surprising. A claimed acute injury may be undermined by an MRI from two years earlier showing the same finding. A “missed” diagnosis may turn out to have been documented but not communicated. A surgical complication may correlate with a known anatomic risk factor that should have changed the operative plan. A persistent symptom may track a pattern that the imaging never captured. Dr. Burnham’s clinical experience as Vice Chair of the Musculoskeletal Service Line and Section Head of Orthopedic Surgery at Ochsner Medical Center — Baton Rouge, combined with team physician work spanning professional sports teams, the University of Pittsburgh, and Southern University, produces the pattern recognition that turns a stack of records into a coherent clinical narrative. The discipline is to build that narrative from the documented findings, not from assumption.
What’s in the Chart: Categories of Records
A complete records review includes every category of clinical documentation that touches the injury at issue and the surrounding medical history. Operative reports are read in full, not summarized; the description of the surgical findings, the techniques used, and the intraoperative complications often contains information that does not appear in the progress notes. Diagnostic imaging is reviewed against the actual images whenever possible, not just the radiology report; an experienced orthopedic reader can identify findings the radiologist did not flag, can quantify the severity of changes the report describes only qualitatively, and can compare studies across time points. Physical therapy notes are reviewed for objective measurements (range of motion, strength, special tests) that often establish the trajectory of recovery more clearly than the surgeon’s office notes. Emergency department records establish the mechanism of injury and the immediate post-injury exam. Primary care and pain management notes capture the longitudinal symptom course and any prior episodes of musculoskeletal complaints relevant to causation analysis.
Prior medical history matters as much as the records of the current claim. A complete review searches for any documentation of pre-existing musculoskeletal conditions that may bear on the causation analysis: prior injuries to the same body part, prior imaging showing degenerative findings, prior surgeries, prior chronic pain workup, occupational exposures that may have contributed to gradual-onset conditions. Charts that appear to document an isolated acute injury sometimes reveal, on careful review, a prior episode that recasts the entire causation question. The reviewer also looks for documentation gaps (records the chart references but does not contain), provider transitions that may have lost information, and inconsistencies between what the patient reported to different providers.
Reading the Imaging: Knowing the Modality Limits
Imaging interpretation is one of the highest-yield areas of records review, in part because every imaging modality has known sensitivity and specificity limits that the unstructured clinical record rarely makes explicit. A radiograph that shows no fracture does not exclude a fracture. An MRI that shows a tear does not establish that the tear is symptomatic. A CT that shows a bony abnormality does not establish that the abnormality caused the patient’s symptoms. The reviewer’s obligation is to know the modality, know its limits, and read the imaging in light of both.
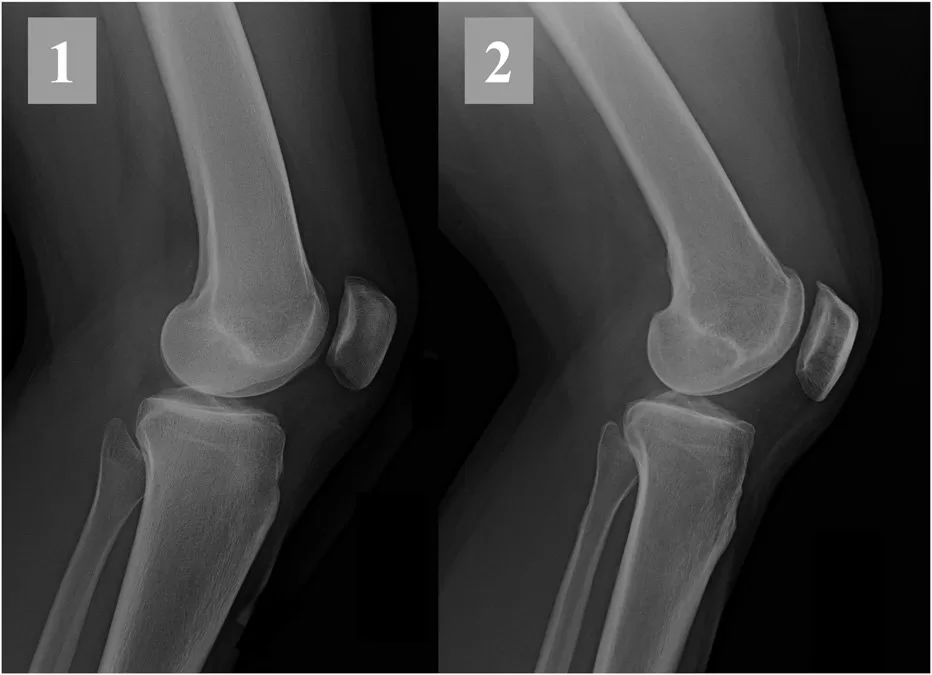
Even the apparently straightforward question of “does this knee have arthritis on plain radiographs” turns out to depend significantly on which view was taken and which grading system was used. Duncan-Burnham et al.’s 2015 systematic review of Level I studies in Arthroscopy found that the 45° flexion posteroanterior (PA) view is more sensitive than the standing anteroposterior (AP) view for detecting severe tibiofemoral osteoarthritis, with no clinical difference in sensitivity between the Kellgren-Lawrence and joint space narrowing grading systems, although the joint space narrowing system may be more specific for ruling in severe medial-compartment osteoarthritis (Duncan-Burnham et al., 2015). The practical implication for records review is straightforward: if the radiographs in the file were obtained with a less-sensitive view, the absence of severe arthritis on those films does not exclude severe arthritis. Reaching that conclusion requires either advanced imaging or a repeat radiographic study with the appropriate technique. A reviewer who does not know the published performance of each radiographic view will read the films at face value and miss the disconnect between what the imaging method can detect and what the clinical question requires.
Imaging Sensitivity for Specific Lesions
The same modality-limits principle applies to MRI, with even greater clinical stakes because MRI is often the imaging modality on which causation and treatment decisions ultimately turn. Different lesions have different MRI detection rates, and the records reviewer must know the published diagnostic performance for each finding at issue. Meniscal ramp lesions of the knee — tears of the posterior meniscocapsular attachment that are clinically important for rotational stability after ACL injury — provide a useful illustration. In a study of 90 patients undergoing ACL reconstruction with arthroscopic confirmation of the diagnosis, Arner, Burnham et al. demonstrated MRI sensitivity for ramp lesions ranging from 53.9% to 84.6%, specificity from 92.3% to 98.7%, negative predictive value from 91.1% to 97.4%, and positive predictive value from 50.0% to 90.0%, with excellent intra-rater reliability (ICC 0.75-0.81) and moderate inter-rater reliability (ICC 0.56) (Arner, Burnham et al., 2017). Ramp lesions were present in 14.4% of the cohort, more frequently than older literature suggested.
The implications for records review are direct. A negative MRI for a ramp lesion does not exclude the lesion, because sensitivity tops out below 85%. A positive MRI is highly likely to be a true positive, because specificity is above 92%. Two readers looking at the same MRI may disagree on the finding, because inter-rater reliability is moderate. None of this is visible in a routine radiology report that simply states “no ramp lesion identified.” When a records reviewer reads the actual MRI images and applies the published diagnostic performance data, the conclusions about what the imaging supports become substantially more defensible. The same logic extends to every category of orthopedic finding for which the published literature has quantified sensitivity, specificity, and reader reliability — rotator cuff tear MRI, labral tear MRI, articular cartilage MRI, occult fracture CT and MRI, and so on. The reviewer who works from the published evidence is positioned to explain in deposition exactly what the imaging supports and where the diagnostic limits lie.
The Imaging-Symptoms Gap
Even when imaging accurately demonstrates a structural abnormality, the imaging finding does not necessarily explain the patient’s symptoms. This imaging-symptoms dissociation is one of the most consequential issues in orthopedic records review, because it bears directly on causation and on whether the proposed treatment is likely to address the actual pain generator. Asymptomatic structural pathology is common across body parts and across populations. Burnham and Bradley’s 2018 editorial commentary in Arthroscopy, addressing recurrent labral tears in National Football League athletes, made the point sharply: among NFL Scouting Combine athletes who had previous labral surgery, recurrent labral tearing was visible on MRI in 32% of shoulders, but those imaging findings showed no relationship to NFL games played or started in the athletes’ rookie year (Burnham & Bradley, 2018). The principle the editorial emphasized — “treat the patient, and not the MRI” — is the principle the records reviewer must apply to every chart that contains an imaging finding offered as the basis for a causation or treatment opinion.
The reviewer’s discipline is to ask whether the imaging finding correlates with the clinical examination, the symptoms the patient reports, the mechanism of injury, and the published natural history of the condition. When imaging and clinical findings align, the causal narrative is straightforward. When they diverge, the divergence itself is the finding. A claimant with a degenerative meniscal tear on MRI but no clinical signs of meniscal pathology and no mechanism consistent with acute meniscal injury may have a tear that exists but does not explain the symptoms. A claimant with normal imaging but persistent objective deficits (weakness, atrophy, abnormal special tests) may have pathology the imaging modality cannot detect at the resolution available. Records review that takes the imaging at face value, without integrating the clinical examination and the published evidence on imaging-symptoms correlation, will produce opinions that the cross-examining attorney can dismantle by reading any one of dozens of asymptomatic-pathology studies into the record.
Timeline Reconstruction and Causation Chains
Beyond imaging, the second high-yield area of records review is the timeline. Most contested orthopedic claims turn on the relationship between events: what happened, when did it happen, what symptoms followed, what imaging was obtained, what diagnoses were made, what treatment was provided, and what was the response. A medical chronology that lays out these events in their actual sequence often resolves causation questions that the unstructured chart obscures. The reviewer assembles the timeline from the records themselves — emergency department visit dates, imaging study dates, surgical dates, physical therapy attendance — and compares it to the narrative in the operative reports, office notes, and any prior depositions or discovery materials.
The patterns that emerge from a well-constructed chronology are often the most consequential findings in the review. A symptom that the claimant reports as starting on the date of injury may, in fact, appear in primary care records from years before. A diagnosis the treating physician characterizes as acute may correspond to an MRI finding that was already present on a study performed for an unrelated complaint. A “delayed” diagnosis may turn out to have been documented at the first visit and then deprioritized as other findings were addressed. A causation chain that the case theory presents as continuous may show a gap of months in which no provider was seen, no symptoms were reported, and no records exist. None of this is visible without the chronology. With the chronology, the medical questions become more answerable, and the eventual opinion becomes more defensible.
Pre-Existing vs. Acute Pathology
The single most contested issue in workers’ compensation and personal injury records review is the distinction between acute traumatic pathology, aggravation of pre-existing degenerative pathology, and entirely pre-existing pathology that is unrelated to the alleged event. The medical literature has documented patterns that allow the reviewer to make principled distinctions in many (though not all) cases. Acute traumatic meniscal tears tend to have specific MRI characteristics that differ from degenerative tears. Acute traumatic rotator cuff tears in younger patients with appropriate mechanisms differ from chronic degenerative tears in older patients with no clear inciting event. Acute traumatic articular cartilage injury differs from osteoarthritic cartilage loss. None of these distinctions is absolute, and the literature supports a degree of clinical judgment in interpreting borderline cases.
The framework Dr. Burnham applies to causation analysis is the same framework the AAOS recommends: identify the causal event, identify the impairment, and assess the probability that the event can cause the impairment, with the threshold most jurisdictions apply being “more probable than not” (greater than 50%) in standard causation cases, though some workers’ compensation jurisdictions apply lower thresholds for aggravation claims (Daniels et al., 2017). The records reviewer’s job is to apply that framework systematically: what is the documented injury mechanism, what is the documented pre-injury condition of the body part, what does the imaging demonstrate about the acute versus chronic character of the pathology, and what does the published natural history of the condition predict about the trajectory the patient would have followed without the alleged event. When all of those questions can be answered from the records, the causation opinion is defensible. When the records do not contain the information needed to answer any one of them, the review documents that gap as well.
Standard of Care vs. Outcome
In medical malpractice records review, the central question shifts from causation to standard of care. The reviewer is not asked whether the event caused the injury; the reviewer is asked whether the care provided met the standard a reasonably competent physician in the same specialty would have provided under the same or similar circumstances. The distinction matters because complications can occur even with appropriate care, and a bad outcome does not, by itself, establish a deviation from the standard of care. The reviewer’s discipline is to evaluate the decision-making process at each stage of treatment: was the diagnostic workup adequate, were the appropriate imaging studies ordered, was the surgical indication appropriate at the time the decision was made, was the surgical technique within the range of accepted practice, was the post-operative management consistent with established protocols.
The standard-of-care analysis must be anchored to what was known at the time of treatment, not what was discovered later. A 2020 surgical decision should be evaluated against the 2020 evidence base, not against later studies that may have changed the recommended approach. Dr. Burnham’s continuous engagement with the evolving evidence base — through more than 145 peer-reviewed publications, current site Principal Investigator roles on the NIH STABILITY 2 and DoD STaR Trials, prior leadership roles with the American Academy of Orthopaedic Surgeons (AAOS), and current participation in the American Orthopaedic Society for Sports Medicine (AOSSM) BOLD Leadership Cohort — provides the methodological grounding to identify which studies were authoritative in the relevant time period and to apply them rigorously. The standard-of-care opinion that survives cross-examination is the one that cites the contemporaneous evidence base and explains its application to the specific decision at issue.
Documentation Standards
The records review report itself is a document attorneys will use, opposing counsel will probe, and (in some contexts) the patient may eventually read. The AAOS-endorsed standard for medicolegal documentation is that the writing should “avoid emotional language and derogatory remarks, not address conditions unrelated to the current claim, and be written so laypeople can understand the rationale” (Daniels et al., 2017). The reviewer’s report should walk the reader through the methodology — what records were reviewed, what imaging was examined, what published literature was consulted — and should connect each conclusion to specific findings in the chart. Unsupported assertions weaken the report. Conclusions that are traceable to the underlying evidence withstand challenge.
The report also distinguishes clearly between what the record establishes, what the record supports as more probable than not, and what the record does not allow the reviewer to determine. Overstating the strength of an opinion is one of the most common reasons records review reports do not survive cross-examination. Acknowledging the limits of the available evidence is not a weakness in the report; it is a marker of methodological rigor that experienced cross-examining attorneys recognize and respect. The opinions the reviewer offers with high confidence are then defensible because they are bounded by the opinions the reviewer declines to offer for lack of evidence.
The Records Review Deliverable
The deliverables a records review engagement produces depend on what the retaining attorney needs. A common starting point is a written records review report that summarizes the materials reviewed, presents the medical chronology, addresses the specific questions the attorney has posed, and offers opinions on each question with the supporting evidence. In some engagements, the report is supplemented or replaced by a verbal opinion conveyed by phone or video conference, which can be appropriate when the attorney needs a rapid assessment before deciding whether to proceed with formal expert development. In litigation that proceeds to discovery, the records review may transition into formal expert witness work, governed by Federal Rule of Civil Procedure 26 in federal cases and analogous state rules elsewhere; for the broader expert witness service offering, see the orthopedic expert witness page.
In addition to the report, attorneys often request a structured medical chronology — a date-ordered table of clinical events with the source of each entry — that they can use as an exhibit, a deposition outline, or a foundation for further discovery requests. When the case involves complex imaging, the reviewer may prepare annotated images or schematic illustrations that explain the relevant findings to a non-medical audience. When the case involves multiple providers, the reviewer may summarize the consistency or divergence of opinions across providers and explain the clinical significance of any disagreements. The deliverable is shaped to the case; the methodology behind it is the same in every engagement.

What Attorneys Should Expect
Attorneys retaining medical records review services through Burnham Orthopedics & Sports Medicine should expect a thorough, methodical engagement. The intake conversation establishes the case type, the medical questions at issue, and the materials available. The reviewer evaluates whether the case falls within the scope of clinical and research expertise and whether there are any conflicts of interest. Once the engagement proceeds, the attorney provides the records, imaging, and any relevant discovery materials, and the reviewer flags any documentation gaps that would be useful to fill before the analysis is finalized. Turnaround time depends on the volume of records, the complexity of the medical questions, and the availability of the imaging studies, but rushed reviews produce reports that do not survive scrutiny; the reviewer will provide a realistic timeline at the outset and communicate proactively if additional time or records are needed.
Attorneys should also expect candor about the strength and limitations of the available evidence. The reviewer who tells the retaining attorney early that a particular position is not supported by the records is more valuable than the reviewer who offers favorable opinions that collapse under cross-examination. When the records do support the retaining party’s position, the report says so clearly. When the records do not, the report says so with equal clarity. The methodology is the same in either direction. Attorneys who use records review as part of an early case assessment, before deposition strategy is set, get the most value from this asymmetry; the review either confirms the case theory and provides the supporting analysis, or it identifies the weaknesses early enough to address them.
About the Author
Jeremy M. Burnham, MD is a board-certified orthopedic surgeon and Vice Chair of the Musculoskeletal Service Line at Ochsner Medical Center — Baton Rouge, Louisiana, providing medical records review and orthopedic expert witness services through Burnham Orthopedics & Sports Medicine. Following his orthopedic surgery residency at the University of Kentucky, he completed his sports medicine fellowship at the University of Pittsburgh Medical Center (UPMC), where he trained under the late Dr. Freddie Fu, a pioneer of anatomic ACL reconstruction, Dr. James Bradley, a renowned sports medicine surgeon and longtime professional team orthopedist, and Dr. Volker Musahl, an internationally recognized ACL surgeon and researcher. His team physician experience spans professional sports teams, the University of Pittsburgh, and Southern University. With more than 145 peer-reviewed publications, book chapters, and scientific presentations, Dr. Burnham is the most published ACL surgeon in Louisiana. His research has been recognized with the Game Changer Award from the Arthritis Foundation and the Playmaker Award from AOSSM. He is a Castle Connolly Top Doctor (peer-nominated), has held previous leadership roles with the American Academy of Orthopaedic Surgeons (AAOS), and is a current member of the AOSSM BOLD Leadership Cohort. He serves as site principal investigator for two federally funded clinical trials (NIH STABILITY 2 and Department of Defense STaR Trial). View full credentials and publications.
The Bottom Line
Medical records review is the foundation on which every credible orthopedic medicolegal opinion is built. Done well, it converts a stack of unstructured records into a coherent clinical narrative that supports defensible opinions on causation, standard of care, treatment necessity, and impairment. Done poorly, it produces opinions that do not survive cross-examination and undermine the case theory they were intended to support. Through Burnham Orthopedics & Sports Medicine, Dr. Burnham offers records review services anchored in more than 145 peer-reviewed publications, book chapters, and scientific presentations; fellowship training at a premier academic center; site Principal Investigator roles on two federally funded clinical trials (NIH STABILITY 2, DoD STaR Trial); hospital leadership roles (Vice Chair, Musculoskeletal Service Line; Section Head, Orthopedic Surgery); and a systematic methodology that emphasizes complete records review, evidence-based imaging interpretation, and clear documentation. Attorneys handling cases involving ACL-related matters in Baton Rouge or broader Gulf South orthopedic claims can review the full scope of Dr. Burnham’s clinical services, research record, and expert witness services before engaging. To discuss a potential records review engagement, contact the office.
Authoritative External Resources
- AAOS Standards of Professionalism — Orthopaedic Surgeon as an Expert Witness
- SEAK, Inc. — Expert Witness Training and Directory
- Federal Rule of Evidence 702 — Testimony by Expert Witnesses
- Federal Rule of Civil Procedure 26 — Duty to Disclose; General Provisions Governing Discovery
- HHS — HIPAA Privacy Rule (governs medical records access in litigation)
References
- Duncan ST, Khazzam MS, Burnham JM, Spindler KP, Dunn WR, Wright RW. Sensitivity of standing radiographs to detect knee arthritis: a systematic review of Level I studies. Arthroscopy. 2015;31(2):321-328. DOI | PubMed | Full-Text PDF
- Arner JW, Herbst E, Burnham JM, et al. MRI Can Accurately Detect Meniscal Ramp Lesions of the Knee. Knee Surg Sports Traumatol Arthrosc. 2017;25(12):3955-3960. DOI | PubMed
- Burnham JM, Bradley JP. Editorial Commentary: MRI Findings Are Only One Part of the Equation in National Football League Athletes: Shoulder Instability in Contact Athletes. Arthroscopy. 2018;34(1):72-73. DOI | PubMed | Full-Text PDF
- Daniels AH, Kuris EO, Palumbo MA. The role of the orthopaedic surgeon in workers’ compensation cases. J Am Acad Orthop Surg. 2017;25(3):e45-e52. DOI | PubMed
Frequently Asked Questions
What is medical records review in legal cases?
Medical records review is a structured analytical exercise in which a qualified physician reads the complete clinical record of a patient or claimant and produces an opinion responsive to specific medical questions, such as causation, treatment appropriateness, impairment, or standard of care. The reviewer is not the treating physician and does not assume care of the patient. The American Academy of Orthopaedic Surgeons (AAOS) framework is explicit that the medicolegal physician’s role is objective evaluation, not treatment (Daniels et al., 2017).
How is records review different from an independent medical examination (IME)?
An IME involves a physical examination of the patient and is governed by state-specific procedural rules in workers’ compensation and insurance contexts. A records review is a paper-and-imaging analysis that may be performed with or without an IME. Many engagements begin with records review alone and only proceed to an IME if the chart raises questions that cannot be resolved without examining the patient. For the IME framework specifically, see the IME for Workers’ Compensation page.
What records does a thorough orthopedic review include?
A complete orthopedic records review includes operative reports read in full (not summarized), diagnostic imaging reviewed against the actual images whenever possible, physical therapy notes for objective measurements, emergency department records establishing mechanism of injury, primary care and pain management notes for the longitudinal symptom course, and any prior medical history that bears on causation analysis. Documentation gaps and provider transitions are flagged. Inconsistencies between what the patient reported to different providers are noted.
Why does the imaging modality matter so much in records review?
Every imaging modality has known sensitivity and specificity limits, and the unstructured clinical record rarely makes those limits explicit. A radiograph that shows no fracture does not exclude a fracture. An MRI that shows a tear does not establish the tear is symptomatic. Different views and grading systems materially change diagnostic performance. For example, the 45° flexion PA radiograph is more sensitive than the standing AP for detecting severe tibiofemoral osteoarthritis (Duncan-Burnham et al., 2015), and MRI sensitivity for meniscal ramp lesions ranges from 53.9% to 84.6% (Arner, Burnham et al., 2017). A reviewer who reads imaging at face value, without the published diagnostic performance data, will produce opinions that do not survive cross-examination.
How do you tell pre-existing pathology from acute injury?
The medical literature has documented patterns that allow principled distinctions in many cases. Acute traumatic meniscal tears tend to have specific MRI characteristics that differ from degenerative tears. Acute traumatic rotator cuff tears in younger patients with appropriate mechanisms differ from chronic degenerative tears in older patients with no clear inciting event. The framework Dr. Burnham applies follows the AAOS recommendation: identify the causal event, identify the impairment, and assess whether the event can cause the impairment “more probable than not,” with some workers’ compensation jurisdictions applying lower thresholds for aggravation claims (Daniels et al., 2017). The records reviewer applies the framework systematically, citing the documented mechanism, pre-injury condition, imaging characteristics, and published natural history.
What does a records review deliverable look like?
Common deliverables include a written records review report (materials reviewed, medical chronology, opinions with supporting evidence), a structured medical chronology that can serve as an exhibit or deposition outline, annotated images or schematic illustrations for non-medical audiences, and a summary of provider consistency or divergence in complex cases. Reports may be supplemented or replaced by a verbal opinion when the attorney needs rapid assessment. The deliverable is shaped to the case; the methodology behind it is the same in every engagement.
How do I retain medical records review services?
The process begins with an initial consultation to discuss the case type, the medical questions at issue, and the materials available. After evaluating scope and conflicts, the engagement proceeds with the attorney providing the records, imaging, and discovery materials. The reviewer flags any documentation gaps useful to fill before analysis is finalized, provides a realistic turnaround timeline, and communicates proactively if additional time or records are needed. To discuss a potential records review engagement with Dr. Burnham, contact Burnham Orthopedics & Sports Medicine.
