What is MPFL Reconstruction
Medial patellofemoral ligament (MPFL) reconstruction is a surgical procedure to help stabilize the patella, or kneecap. The MPFL is a ligament on the inside of the knee that connects the end of the femur (thigh bone) to the patella (kneecap). It serves as a check rein on the kneecap and prevents it from moving too far to the outside of the knee.
In cases of patella dislocation or recurrent patellar instability, the MPFL can become torn or stretched out. Although non-surgical management is usually the first line of treatment, sometimes reconstruction of the torn or stretched ligament is needed. As Dr. Burnham has emphasized, treating patients with recurrent patellar instability requires an individualized, anatomic approach, much like the evolution seen in ACL reconstruction.
Why is MPFL Reconstruction Surgery Performed
Reconstruction of the MPFL is performed when the ligament is stretched or torn due to repeated or severe dislocation of the patella. Although non-surgical treatment with a physical therapist, knee braces, and muscle strengthening are usually tried first, some tears of the MPFL will not heal sufficiently on their own.
Many factors lead to patellar instability. Some of these can be corrected and some cannot. Modifiable and non-modifiable risk factors must be assessed before deciding on definitive treatment. Sometimes a repair of the torn ligament is adequate, but replacing or reconstructing the ligament is shown to have improved outcomes compared to repair in most situations.
MPFL reconstruction is one of the most common procedures utilized when surgery is needed to stabilize the patella.
Who Needs MPFL Reconstruction?
Not every patient with a dislocated kneecap needs MPFL reconstruction surgery. The decision depends on several patient-specific factors that an orthopedic surgeon evaluates during a thorough clinical workup. Candidates for MPFL reconstruction typically include patients who meet one or more of the following criteria:
Recurrent patellar dislocations. Patients who have experienced two or more episodes of kneecap dislocation are strong candidates for surgery. After the first dislocation, the risk of a second episode is approximately 15 to 40 percent, and that risk climbs significantly with each subsequent dislocation. When the kneecap keeps dislocating despite bracing and physical therapy, surgical stabilization offers the most reliable path to long-term stability.
First-time dislocation with significant risk factors. In some cases, even a first-time dislocation may warrant surgical discussion. Patients with anatomic risk factors such as trochlear dysplasia (a shallow groove for the kneecap), patella alta (a high-riding kneecap), an elevated TT-TG distance (a measurement indicating the kneecap’s pull is shifted too far laterally), or significant knee valgus (knock knees) may benefit from earlier surgical intervention. A systematic review by Burnham et al. found that addressing these anatomic factors, sometimes with concomitant procedures such as a tibial tubercle transfer, improves outcomes and reduces redislocation rates.
Young, active athletes. Athletes who need to return to cutting, pivoting, and contact sports place high demands on knee stability. For these patients, the combination of a torn MPFL and the physical requirements of their sport often tips the scale toward reconstruction.
Failed non-surgical treatment. Patients who have completed a structured physical therapy program focused on quadriceps and hip strengthening but continue to experience instability episodes, apprehension, or giving-way symptoms are candidates for surgical stabilization.
Loose bodies or cartilage damage. When a patellar dislocation causes a piece of cartilage or bone to break off inside the knee joint, surgical intervention is often necessary to remove the loose body and address the underlying instability simultaneously.
Video Overview of MPFL Recon
How is Medial Patellofemoral Ligament Reconstruction Performed
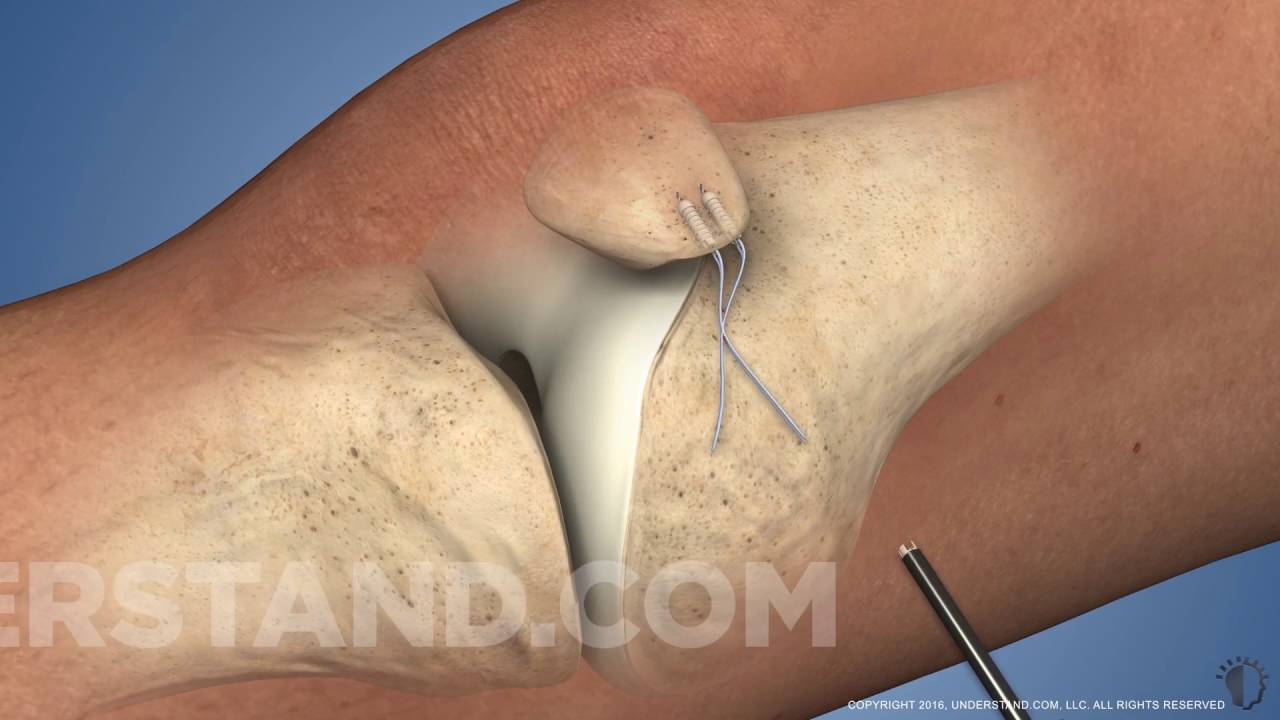
Reconstruction of the medial patellofemoral ligament is performed by replacing the torn or stretched ligament with a new one. Sources of the new ligament are varied. This can include the patient’s own hamstring tendon, or autograft. Allograft is tissue from a cadaver, or someone who donated their body to medicine. This is commonly used to make a new MPFL.
The new ligament is attached on the medial, or inside of the knee cap. It is then routed through the soft tissues to the place where it attaches on the femur. The native MPFL attaches on the medial femoral condyle. X-ray is often used to help locate the correct attachment site, known as Schottle’s point.
The knee is then brought through range of motion testing, and the graft is tensioned to ensure that it serves as a check rein preventing the kneecap from dislocating, but also to make sure it does not put undue pressure on the knee joint. The goal is to have normal patellar tracking without the MPFL graft pulling the kneecap too far to the medial side.
MPFL Surgery Recovery Timeline
Recovery after MPFL reconstruction follows a structured, phased protocol designed to protect the reconstructed ligament while progressively restoring range of motion, strength, and function. Every patient’s timeline varies slightly depending on whether additional procedures (such as a tibial tubercle transfer or cartilage procedure) were performed at the same time, but the general framework follows the milestones below.
Day of surgery (Day 0). MPFL reconstruction is performed as an outpatient procedure, meaning patients go home the same day. A nerve block is administered before surgery to manage pain for the first 12 to 24 hours. Patients leave the surgical center with crutches, a knee brace locked in extension, and specific instructions for icing and elevation.
Weeks 1 to 2. The focus during the first two weeks is on controlling swelling and managing pain. The knee brace is worn at all times, and patients remain partial weight bearing with crutches. Gentle range of motion exercises, quad sets, and straight leg raises begin immediately under the guidance of a physical therapist. Most patients can return to light desk work within 1 to 2 weeks.
Weeks 2 to 6. Progressive range of motion is the primary goal during this phase. Patients work toward achieving 90 degrees of flexion by week 4 and full flexion by week 6. Weight bearing is gradually increased as tolerated. The knee brace may be unlocked for controlled range of motion exercises. Gluteal and quadriceps strengthening exercises continue to build the muscular support around the knee.
Weeks 6 to 12. The stationary bike is introduced around week 6, which helps restore range of motion and build endurance. Patients transition off crutches as their strength and gait normalize. Closed-chain strengthening exercises such as leg presses, step-ups, and mini squats are introduced. The brace is typically discontinued during this phase.
Months 3 to 4. Functional progression begins, including balance and proprioception training. Patients start light jogging on flat surfaces when adequate quadriceps strength is demonstrated (typically when the operative leg reaches 70% or more of the strength of the non-operative leg). Sport-specific movement patterns are introduced gradually.
Months 4 to 6. Advanced sport-specific training begins, including cutting, pivoting, and agility drills. Patients must demonstrate adequate strength, stability, and confidence before progressing to contact activities. Functional testing is performed to objectively measure readiness for return to sport.
Months 6 to 9 (return to sport). According to a systematic review published in the American Journal of Sports Medicine, the average time to return to sport after MPFL reconstruction is 6.7 months. Return-to-sport decisions are based on objective functional testing, not simply the calendar. Athletes must pass sport-specific testing criteria before being cleared for full, unrestricted competition.
View the MPFL Postoperative Protocol for physical therapy here.
MPFL Reconstruction Success Rate
Medial patellofemoral ligament surgery has been researched extensively. A systematic review and meta-analysis published in AJSM found that 92.8% of patients were able to return to sports after MPFL reconstruction. Furthermore, 71.3% of patients returned to or surpassed their preoperative activity level.
The overall complication rate was 8.8%. The most common complication was recurrent instability (1.9%).
A systematic review by Burnham et al. examining MPFL reconstruction with concomitant tibial tubercle transfer found that addressing multiple anatomic risk factors simultaneously can further improve outcomes in patients with complex patellar instability. The key is matching the surgical plan to each patient’s unique anatomy, a principle Dr. Burnham has advocated for in the orthopedic literature.
MPFL Surgery Alternatives
Surgery is not always the first step in treating patellar instability. Several non-surgical and surgical alternatives to MPFL reconstruction exist, and the right approach depends on the severity and frequency of instability, the patient’s anatomy, and their activity goals.
Physical therapy and bracing. For first-time dislocations without significant structural risk factors, a structured physical therapy program is typically the first-line treatment. Therapy focuses on strengthening the quadriceps (especially the VMO, or vastus medialis oblique), the hip abductors, and the core. A patellar stabilizing brace may be used during activity to provide additional support while the muscles rebuild. Many patients achieve satisfactory stability through therapy alone.
MPFL repair. In select cases where the MPFL is torn at a specific location (usually from the kneecap), a repair rather than a full reconstruction may be appropriate. Repair involves reattaching the native ligament tissue using surgical anchors and sutures. However, reconstruction is generally preferred when the ligament is stretched or attenuated rather than cleanly torn, as reconstruction provides a stronger, more reliable restraint.
Tibial tubercle transfer (osteotomy). In patients with an elevated TT-TG distance or patella alta, a tibial tubercle osteotomy may be performed either as a standalone procedure or in combination with MPFL reconstruction. This procedure repositions the attachment point of the patellar tendon on the tibia to improve patellar tracking. Research by Burnham et al. has examined outcomes when these procedures are combined.
Trochleoplasty. For patients with severe trochlear dysplasia (a flat or convex femoral groove), trochleoplasty reshapes the groove to better accommodate the kneecap. This is a more involved procedure reserved for significant anatomic abnormalities and is often combined with MPFL reconstruction.
Frequently Asked Questions About MPFL Surgery
Is MPFL reconstruction major surgery?
Yes, medial patellofemoral ligament reconstruction is considered a “major” surgery. It requires general anesthesia, and a portion of the surgery requires open incisions. However, it is performed as an outpatient procedure, which means patients go home the same day. It typically requires only two small incisions.
How painful is MPFL reconstruction surgery?
It is normal to have pain after MPFL surgery, especially on the inside of the knee. The pain usually starts to noticeably improve 1 to 2 weeks after surgery, though some discomfort may persist for 3 to 4 months. A nerve block is usually administered prior to surgery, which typically lasts for the day of surgery. Pain medications are prescribed to help manage discomfort after the nerve block wears off.
What is MPFL reconstruction?
MPFL reconstruction is a surgical procedure to replace a damaged or stretched medial patellofemoral ligament. This ligament acts as a check rein on the kneecap, preventing it from sliding too far to the outside of the knee. The surgery stabilizes the knee and prevents recurrent patellar dislocation.
How long is MPFL reconstruction surgery?
The surgery to reconstruct the medial patellofemoral ligament usually takes between 1 to 2 hours, depending on the complexity of the case. Sometimes additional procedures are performed at the same time, such as cartilage restoration or a tibial tubercle osteotomy (in cases of elevated TT-TG distance), which may extend the surgical time.
How long is MPFL surgery recovery time?
Full recovery from MPFL reconstruction typically takes 6 to 9 months. Most patients can return to desk work within 1 to 2 weeks, begin riding a stationary bike around week 6, and start light jogging between months 3 and 4. The average return to sport is 6.7 months, according to a systematic review in the American Journal of Sports Medicine. Return-to-sport decisions are based on objective functional testing, not simply the calendar.
Can you walk after MPFL reconstruction surgery?
Patients are able to walk with crutches and a knee brace immediately after MPFL surgery. For the first 4 to 6 weeks, patients are kept partial weight bearing with crutches to protect the healing graft. Most patients transition off crutches between weeks 6 and 12 as their strength and gait normalize. Walking without any assistive devices is typically achieved by 2 to 3 months after surgery.
What is the MPFL reconstruction success rate?
MPFL reconstruction has a high success rate. Research shows that 92.8% of patients return to sports after the procedure, and 71.3% return to or exceed their pre-injury activity level. The overall complication rate is 8.8%, with the most common complication being recurrent instability at just 1.9%. Outcomes improve further when the surgical plan is tailored to each patient’s specific anatomy.
How much time do I need to take off from work after MPFL surgery?
Most patients can return to light duty or seated work within 1 to 2 weeks after medial patellofemoral ligament reconstruction. Return to physically demanding work will vary depending on specific job requirements. The timeline for return to heavy labor is individualized based on the surgery performed and the physical demands of the job.
What is the difference between MPFL repair and MPFL reconstruction?
MPFL repair involves reattaching the torn native ligament back to the bone using surgical anchors and sutures. This is best suited for acute, localized tears. MPFL reconstruction involves replacing the entire damaged ligament with new tissue, either from the patient (autograft) or from a donor (allograft). Reconstruction is generally preferred for recurrent instability or when the ligament is stretched out rather than cleanly torn, as it provides more reliable long-term stability.
Are there alternatives to MPFL surgery?
Yes. For first-time patellar dislocations without significant anatomic risk factors, non-surgical treatment with physical therapy, quadriceps strengthening, and patellar stabilizing braces is typically the first approach. Many patients achieve satisfactory stability without surgery. However, patients with recurrent dislocations, significant cartilage damage, or anatomic risk factors (trochlear dysplasia, patella alta, elevated TT-TG distance) are more likely to benefit from surgical stabilization.
Is it normal to have numbness after MPFL surgery?
Some numbness around the incision site is normal after MPFL surgery. This is caused by small superficial branches of the saphenous nerve that run near the surgical site. The numbness typically improves over several months as the nerves heal, though a small area of altered sensation may persist long-term in some patients.
When can I drive after MPFL reconstruction?
Most patients can resume driving 4 to 6 weeks after MPFL reconstruction, depending on which leg was operated on and whether they drive an automatic or manual transmission. Patients who had surgery on the left knee and drive an automatic vehicle may be able to drive sooner, sometimes within 2 to 3 weeks, as long as they are no longer taking narcotic pain medications and feel confident controlling the vehicle safely.
MPFL Reconstruction in Baton Rouge, Louisiana
Dr. Jeremy Burnham is a board-certified orthopedic surgeon and sports medicine specialist at Ochsner-Andrews Sports Medicine Institute in Baton Rouge, Louisiana. With peer-reviewed research specifically focused on MPFL reconstruction and patellar instability, Dr. Burnham brings an evidence-based, individualized approach to every patient. The surgical team treats patients from across Baton Rouge, Gonzales, Denham Springs, Hammond, Lafayette, and throughout Louisiana.
About the Author
Dr. Jeremy Burnham is a board-certified, fellowship-trained orthopedic surgeon and sports medicine specialist at Ochsner-Andrews Sports Medicine Institute in Baton Rouge, Louisiana. He completed orthopedic residency at the University of Kentucky and sports medicine fellowship at the University of Pittsburgh Medical Center under Drs. Freddie Fu, Volker Musahl, and James Bradley. Dr. Burnham is one of the highest-volume knee surgeons and most-published sports medicine researchers in Louisiana, with 53 peer-reviewed publications, 13 book chapters, and 61 podium and poster presentations.
Clinical focus: ACL reconstruction, complex and revision knee reconstruction, patellar instability and MPFL reconstruction, cartilage restoration, meniscus repair, and sports injury care. Full biography · Research and publications
References
- Platt BN, Bowers LC, Magnuson JA, Marx SM, Liu JN, Farr J, Stone AV. Return to Sport After Medial Patellofemoral Ligament Reconstruction: A Systematic Review and Meta-analysis. Am J Sports Med. 2022 Jan;50(1):282-291. doi: 10.1177/0363546521990004. Epub 2021 Mar 15. PMID: 33720789.
- Burnham JM. Editorial Commentary: Treating Patients With Recurrent Patellar Instability With an Individualized, Anatomic Approach Is Needed: Learn From the Anterior Cruciate Ligament. Arthroscopy. 2021 May;37(5):1680-1682. doi: 10.1016/j.arthro.2021.01.018. PMID: 33896516.
- Burnham JM, Howard JS, Hayes CB, Lattermann C. Medial Patellofemoral Ligament Reconstruction With Concomitant Tibial Tubercle Transfer: A Systematic Review of Outcomes and Complications. Arthroscopy. 2016 Jun;32(6):1185-95. doi: 10.1016/j.arthro.2015.11.039. Epub 2016 Feb 13. PMID: 26882966.
