BioUni Knee Cartilage Reconstruction
Knee cartilage replacement technique with osteochondral allograft (OATS)
Osteochondral Allograft Transplantation to Replace Damaged Cartilage in the Knee
Large defects in the cartilage do not cartilage do not heal on their own, and will get larger with time. The Arthrex BioUni procedure utilizes a fresh cartilage and bone graft from donor tissue to replace or reconstruct cartilage defects on on the inside, or medial aspect, of the knee.
What is the BioUni?
Arthrex BioUni is an osteochondral allograft transplantation procedure that can be used to treat patients with large, full-thickness cartilage defects of the knee. The BioUni utilizes special instrumentation that allows reconstruction of larger knee cartilage defects.
What are the differences between BioUni and Knee Replacement?
The BioUni' name is similar to a partial, or "unicompartmental" knee replacement. However, the BioUni replaces your damaged cartilage with cartilage from a donor, while knee replacement replaces the damaged cartilage with artificial materials (metal and plastic).
See if You qualify for Cartilage Reconstruction
See if You qualify for Knee Cartilage Reconstruction
HIGHLIGHTS of
BioUni Knee Cartilage Reconstruction Surgery
Useful for Large or Irregularly Shaped Cartilage Defects
Some lesions are too large or too oval-shaped for other forms of cartilage restoration surgery. The BioUni instrumentation allows harvesting of large and oval shaped grafts from the donor tissue. While other cartilage procedures such as micro fracture can't recreate the same type of cartilage tissue, BioUni results in healthy hyaline articular cartilage.
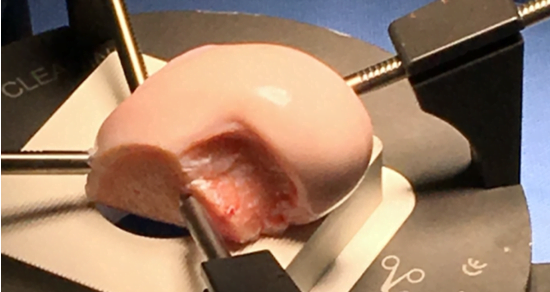

Elite Level Surgical Care
The Ochsner-Andrews Sports Medicine Institute team in Baton Rouge, LA specializes in surgical treatment of complex knee injuries, including cartilage reconstruction surgery. Dr. Burnham is an orthopedic surgeon and knee doctor who specializes in complex "non-knee replacement" knee surgery such as cartilage reconstruction.
Return to an Active Lifestyle after Cartilage Surgery
Injuries to the articular cartilage cause pain, swelling, and loss of function. Eventually, they lead to bone-on-bone arthritis. Cartilage reconstruction procedures like BioUni can reconstruct the damaged knee joint cartilage and help patients return to sports.

Why choose us?
Reviews of Dr. Burnham and Team
"Dr. Burnham is amazing. I had a traumatic knee injury that he performed surgery on...he does A+ work. With an injury like this you want the best, and Dr. Burnham is the best. I highly recommend him."
Marie
Verified Google Review
Individualized, patient-centered approach
Every patient is an individual. Our team works together to develop a patient-focused treatment plan. There is no "one-size-fits-all" cartilage surgery.
BOARD CERtified & Fellowship-trained
Dr. Jeremy Burnham is certified in Orthopedic Surgery and in Orthopedic Sports Medicine by the American Board of Orthopedic Surgery (ABOS). His main location is in Baton Rouge, LA and Hammond, LA, while servicing surrounding areas (Lafayette, Prairieville, Gonzales, Zachary, Central, Denham Springs, Walker, Livingston Parish, Brusly, Port Allen, St. Francisville, and New Roads).
Multi-disciplinary regenerative medicine team
The Ochsner Sports Medicine Institute features experts in knee surgery including knee joint cartilage repair and cartilage reconstruction procedures.
Patient Indications for BioUni Surgical Procedure
Potential Candidates for BioUni:
Potential Contraindications for BioUni:
Dr. Jeremy Burnham is a board-certified orthopedic surgeon who specializes in the surgical treatment of complex knee injuries. His clinical and research focus is centered around diagnosis and treatment of knee conditions.
Dr. Burnham is the team physician for Southern University, the Baton Rouge Rougarou minor league baseball, and several area high schools. He is the principle investigator for research studies examining the best treatment techniques for knee injuries.
Jeremy M. Burnham, MD

FAQ. Frequently Asked Questions
The traditional form of cartilage replacement in the knee is called a "knee replacement." This involves replacing damaged cartilage and bone in the knee with synthetic materials (various mixes of plastic and metal). Knee replacement is usually performed in cases of diffuse arthritis and cartilage damage (damage in 2 or more of the 3 compartments in the knee).
In some cases of isolated cartilage defects, more localized cartilage procedures can be performed. One example of this is the Arthrex BioUni osteochondral allograft transplantation. This procedure uses the bone and cartilage from donated tissue (i.e. allograft, or cadaver tissue) to replace the damaged area of bone and cartilage. The body then incorporates the cartilage graft as it's own cartilage and bone.
Research studies have shown that osteochondral allografts show survivorship of over 80% at 5 years. The longevity of the grafts has shown to be lower in patients aged 40 years or older, and in overweight patients. Patients with a body mass index (BMI) of >35 were shown to have a 4 times greater risk of graft failure than those with lower body weight at 5 year follow-up. However, at 2-year follow-up, there were no differences in graft survival based on BMI.
Knee replacement surgery is also known as knee arthroplasty. This procedure involves replacing the damaged cartilage and bone in your knee with artificial materials. It’s usually performed when you have diffuse arthritis, which is damage in two or more of the three compartments in your knee.
In some cases of isolated cartilage defects, more localized procedures can be performed. One example is the Arthrex BioUni osteochondral allograft transplantation. This uses bone and cartilage from donated tissue (allograft or cadaver tissue) to replace the damaged area of bone and cartilage. The body then incorporates the cartilage graft as its own cartilage and bone.
You will be limited, or non-weight bearing for the first 6-8 weeks after your surgery. You will also wear a knee brace that helps stabilize and protect the knee.
From weeks 8-12, you will focus on walking normally and early strengthening. You will focus on functional strength and cardiovascular fitness from weeks 12-20.
After week 20, you will start working on functional activities and getting ready for return to sport. All patients are advised to stick to low impact activities only for the first 12 months. Full return to sports depends on the sport played, milestones reached during rehab, and time from surgery.
