GLP-1 receptor agonists like semaglutide (Ozempic, Wegovy) and tirzepatide (Mounjaro, Zepbound) have transformed weight management. The clinical results are unprecedented, with patients achieving 15 to 21% total body weight reduction in landmark trials. But as these medications become the standard of care for obesity, an important question is emerging from the orthopedic and musculoskeletal literature: what happens to bone density and lean muscle mass during rapid, pharmacologically driven weight loss?
The answer, based on recent randomized controlled trial data, is that the skeletal cost of GLP-1 therapy deserves serious attention. A 2024 phase 2 RCT by Hansen et al. (eClinicalMedicine) found that 52 weeks of once-weekly semaglutide reduced hip bone mineral density by 2.6% and lumbar spine density by 2.1% compared to placebo, with increased bone resorption and no compensatory increase in bone formation. Separately, the SURMOUNT-1 DXA substudy by Look et al. (Diabetes, Obesity and Metabolism, 2025) showed that tirzepatide reduced total lean mass by 10.9% over 72 weeks. These findings do not mean GLP-1 medications should be avoided. They mean that prescribing them without a musculoskeletal protection plan is incomplete care.

What GLP-1s Do to Bone: The Hansen Trial
The most rigorous bone-specific data on GLP-1 therapy comes from Hansen et al. (eClinicalMedicine, 2024), a randomized, double-blinded, two-centre, phase 2 trial of once-weekly semaglutide 1.0 mg versus placebo in 64 adults with increased fracture risk. This was not a post-hoc analysis or observational study. It was designed specifically to measure skeletal outcomes.
At 52 weeks, the semaglutide group showed a statistically significant reduction in areal bone mineral density at the total hip (estimated treatment difference: -0.020 g/cm², p = 0.001, equating to approximately 2.6% loss) and at the lumbar spine (ETD: -0.018 g/cm³, p = 0.007, approximately 2.1% loss). For context, postmenopausal women typically lose 1 to 2% of hip BMD per year. A 2.6% reduction in a single year of semaglutide therapy on top of that baseline rate is clinically meaningful, particularly for patients who are already in an at-risk category.
The trial also used high-resolution peripheral quantitative CT (HR-pQCT) to evaluate bone microarchitecture. Tibial cortical thickness decreased by 1.8% (p = 0.012) in the semaglutide group. Body weight in the semaglutide group decreased by an estimated 6.8 kg more than placebo, confirming the expected weight loss effect, but the bone changes occurred in parallel rather than being fully explained by mechanical unloading from weight loss alone.
The Lean Mass Problem: SURMOUNT-1 DXA Data
Bone density is only part of the picture. The composition of weight loss, specifically how much of it is fat versus muscle, matters enormously for long-term musculoskeletal health. The SURMOUNT-1 DXA substudy by Look et al. (Diabetes, Obesity and Metabolism, 2025) provided the most detailed body composition data available on GLP-1/GIP dual receptor agonist therapy.
Over 72 weeks, tirzepatide (15 mg dose) reduced total fat mass by 33.9% versus 8.2% with placebo. That is a substantial and clinically meaningful fat reduction. However, lean body mass also decreased by 10.9% in the tirzepatide group versus 2.6% with placebo. The proportion of weight loss held at roughly 75% fat and 25% lean mass, which is consistent with diet-induced weight loss in general. But when total weight loss exceeds 20%, as it does in many GLP-1/GIP patients, that 25% lean mass fraction represents a significant absolute deficit in muscle tissue.
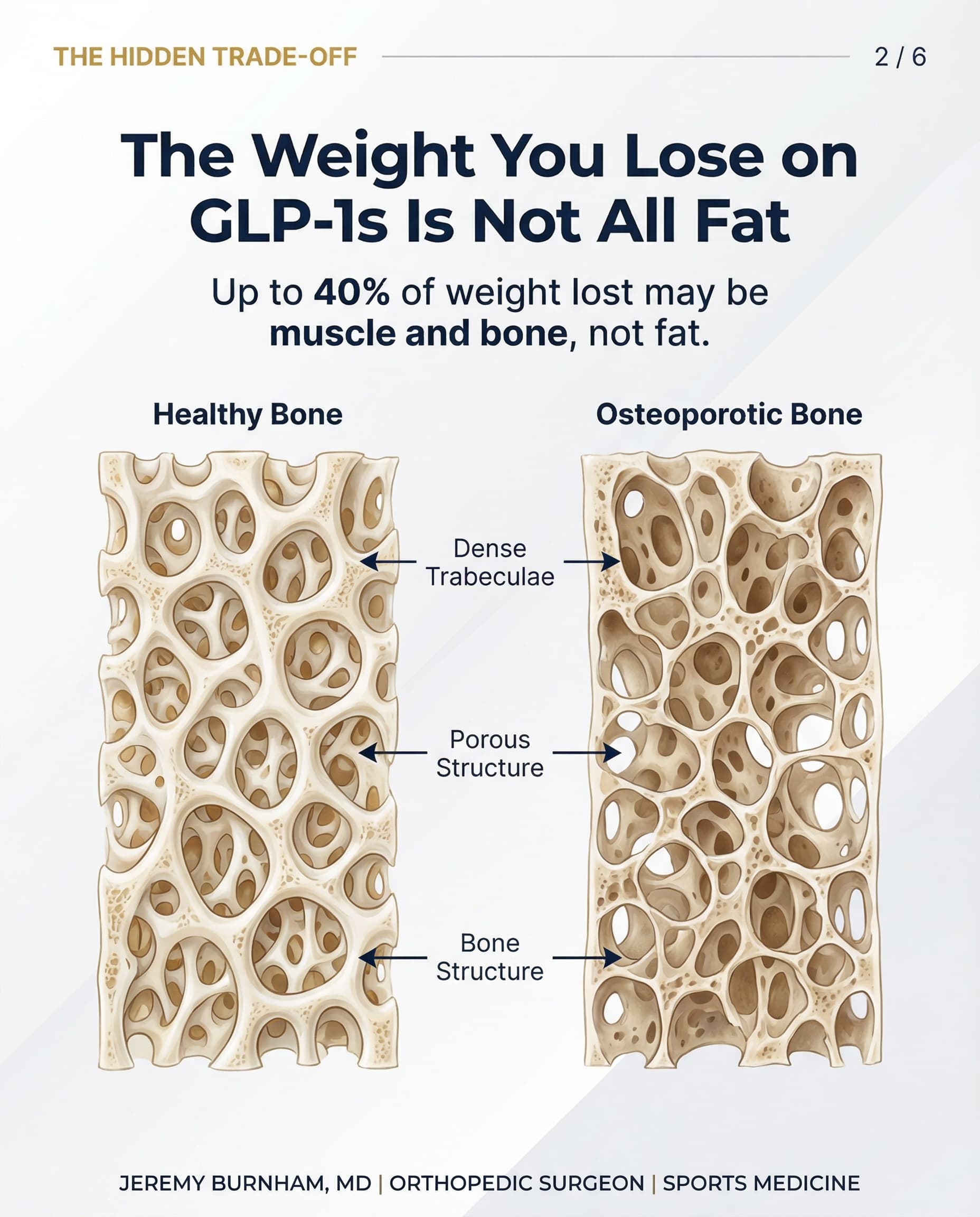
For an orthopedic surgeon, this is relevant because muscle mass is a primary driver of joint stability, injury prevention, and post-surgical recovery. Patients who present for ACL reconstruction, knee replacement, or any lower extremity procedure with significant sarcopenia (muscle loss) have longer recovery timelines and worse functional outcomes. Approximately 25% of the weight lost on tirzepatide was lean mass rather than fat, and in semaglutide trials (STEP 1 DXA subset), that proportion may approach 40%. Patients need to understand that distinction.

Who Is Most at Risk
Not every patient on a GLP-1 faces the same level of skeletal risk. The patients Dr. Burnham’s team at Ochsner-Andrews Sports Medicine Institute are most concerned about are those with multiple overlapping risk factors. The cumulative risk is what matters.
Post-menopausal women are at the top of the list. Estrogen decline already accelerates bone resorption, and the Hansen trial specifically enrolled adults with increased fracture risk. Adding a medication that further reduces BMD compounds an existing vulnerability. Adults over 50 face similar concerns, as age-related bone loss is already underway and the ability to rebuild lost bone becomes progressively more limited.
Patients losing weight rapidly (more than 1 to 2 pounds per week sustained over months) are at higher risk because the mechanical unloading signal to bone is more acute. Sedentary patients who are not performing resistance training lose both the osteogenic stimulus that weight-bearing exercise provides and the muscle mass that protects joints. And patients with inadequate protein intake cannot adequately support muscle protein synthesis during a catabolic weight loss phase, accelerating the lean mass deficit.
When multiple risk factors overlap in a single patient (for example, a 55-year-old post-menopausal woman who is sedentary and losing weight rapidly on semaglutide without a structured exercise program), the conversation about bone and muscle protection becomes essential, not optional.

Understanding the Bone Turnover Data
One of the most important findings from the Hansen trial is the pattern of bone turnover markers. In healthy bone metabolism, bone resorption (the breakdown of old bone) and bone formation (the building of new bone) are coupled. When resorption increases, formation typically increases in response, maintaining overall bone balance. The semaglutide data showed an uncoupling of this process.
P-CTX (procollagen type I C-terminal cross-linked telopeptide), a marker of bone resorption, increased significantly in the semaglutide group compared to placebo (p = 0.021). P-PINP (procollagen type I N-terminal propeptide), a marker of bone formation, did not show a compensatory increase. This means bone was being broken down faster without being rebuilt at a matching rate, a pattern that, if sustained, leads to net bone loss over time.
This uncoupling is clinically relevant because it suggests the bone density changes seen in the Hansen trial are not simply a transient effect of weight loss but may reflect a direct or indirect metabolic effect of GLP-1 receptor activation on bone turnover. Whether this pattern persists beyond 52 weeks, whether it is dose-dependent, and whether it is reversible upon discontinuation of therapy are questions that remain unanswered and need to be addressed in larger, longer-duration trials.
Four Non-Negotiables for Bone and Muscle Protection
The evidence points clearly toward a set of protective interventions that should accompany any GLP-1 prescription. These are not optional add-ons. For patients at risk, they are foundational to safe weight loss.
Resistance training at least three times per week with compound movements. Exercises like squats, deadlifts, lunges, and presses create the mechanical loading signal that drives bone formation and maintains muscle mass during caloric deficit. A meta-analysis in Scandinavian Journal of Medicine and Science in Sports confirmed that energy deficiency impairs resistance training gains in lean mass, and that individuals performing resistance training to preserve lean mass during weight loss should avoid energy deficits greater than 500 kcal/day (Murphy & Koehler, Scand J Med Sci Sports, 2022). Without structured resistance training, the 25% lean mass loss fraction may increase further.
Protein intake of 1.2 to 1.6 grams per kilogram of body weight per day. This range is recommended by ESPEN (European Society for Clinical Nutrition and Metabolism) and PROT-AGE guidelines for older adults and patients in catabolic states. During GLP-1 therapy, when appetite is suppressed and total caloric intake is reduced, hitting adequate protein becomes both harder and more important. Protein provides the amino acid substrate necessary for muscle protein synthesis, and inadequate intake during weight loss directly accelerates sarcopenia.
Calcium (1,000 to 1,200 mg daily) and Vitamin D3 (1,500 to 2,000 IU daily). These are baseline requirements for bone health that become especially important when bone resorption markers are elevated, as demonstrated in the Hansen trial. Many patients on GLP-1 therapy are eating less overall, which means dietary calcium intake may drop below the threshold needed for bone maintenance. Supplementation fills that gap.
A baseline DXA scan before or soon after starting GLP-1 therapy. A DXA scan provides an objective measurement of bone mineral density at the hip and lumbar spine, the same sites where the Hansen trial documented losses. Having a baseline measurement allows the prescribing team to monitor for clinically significant changes over time and adjust the protection plan accordingly. For patients with pre-existing osteopenia or osteoporosis, a baseline DXA may change the risk-benefit calculation of GLP-1 therapy entirely.

About the Author
Jeremy M. Burnham, MD is a board-certified orthopedic surgeon and Director of Sports Medicine at Ochsner-Andrews Sports Medicine Institute in Baton Rouge, Louisiana. Following his orthopedic surgery residency at the University of Kentucky, he completed his sports medicine fellowship at the University of Pittsburgh Medical Center (UPMC), where he trained under the late Dr. Freddie Fu, a pioneer of anatomic ACL reconstruction, Dr. James Bradley, a renowned sports medicine surgeon and longtime professional team orthopedist, and Dr. Volker Musahl, an internationally recognized ACL surgeon and researcher. His team physician experience spans professional sports teams, the University of Pittsburgh, and Southern University. With 127 peer-reviewed publications, book chapters, and scientific presentations, Dr. Burnham is the most published ACL surgeon in Louisiana. His research focuses on advancing ACL reconstruction, optimizing return-to-sport outcomes, and pioneering injury prevention, and has been recognized with the Game Changer Award from the Arthritis Foundation and the Playmaker Award from AOSSM. He serves as a site principal investigator for two federally funded clinical trials (NIH STABILITY 2 and Department of Defense STaR Trial). View full credentials and publications.
The Bottom Line
GLP-1 receptor agonists are among the most effective weight loss medications ever developed. The metabolic benefits for patients with obesity, type 2 diabetes, and cardiovascular risk are well established and continue to expand with ongoing research. Nothing in this article should be read as discouraging their use where clinically indicated.
But the musculoskeletal data is real and cannot be ignored. A 2.6% reduction in hip bone mineral density and a 2.1% reduction at the lumbar spine in 52 weeks (Hansen et al., 2024), combined with up to 10.9% lean mass loss over 72 weeks (Look et al., 2025), means that patients on GLP-1 therapy need a comprehensive musculoskeletal protection plan from day one. Resistance training, adequate protein, calcium and vitamin D3 supplementation, and baseline DXA screening are not extras. They are the standard of care for safe, sustainable weight loss on these medications. The patients who do best on GLP-1 therapy are the ones who have a plan to protect their bones and muscle from the start.

References
- Hansen MS, Wolfel EM, Jeromdesella S, Moller JJK, Ejersted C, Jorgensen NR, Eastell R, Hansen SG, Frost M. “Once-weekly semaglutide versus placebo in adults with increased fracture risk: a randomised, double-blinded, two-centre, phase 2 trial.” eClinicalMedicine. 2024;72:102624. PMID: 38737002 | DOI
- Look M, Dunn JP, Kushner RF, Cao D, Harris C, Gibble TH, Stefanski A, Griffin R. “Body composition changes during weight reduction with tirzepatide in the SURMOUNT-1 study of adults with obesity or overweight.” Diabetes, Obesity and Metabolism. 2025;27(5):2720-2729. PMID: 39996356 | DOI
- Murphy C, Koehler K. “Energy deficiency impairs resistance training gains in lean mass but not strength: a meta-analysis and meta-regression.” Scandinavian Journal of Medicine and Science in Sports. 2022;32(1):125-137. PMID: 34623696 | DOI
- Jastreboff AM, Aronne LJ, Ahmad NN, Wharton S, Connery L, Alves B, Kiyosue A, Zhang S, Liu B, Bunck MC, Stefanski A. “Tirzepatide once weekly for the treatment of obesity.” New England Journal of Medicine. 2022;387(3):205-216. PMID: 35658024 | DOI
Frequently Asked Questions
Do GLP-1 medications like Ozempic cause bone loss?
A 2024 randomized controlled trial by Hansen et al. found that 52 weeks of once-weekly semaglutide (the active ingredient in Ozempic and Wegovy) reduced hip bone mineral density by 2.6% and lumbar spine density by 2.1% compared to placebo in adults with increased fracture risk. Bone resorption markers increased while bone formation markers did not compensate. This suggests a real, measurable effect on bone that warrants monitoring and protective interventions, particularly for patients who are already at risk for osteoporosis.
How much muscle do you lose on semaglutide or tirzepatide?
The SURMOUNT-1 DXA substudy (Look et al., 2025) showed that tirzepatide reduced lean body mass by 10.9% over 72 weeks, compared to 2.6% with placebo. The proportion of weight loss was approximately 75% fat and 25% lean mass. Approximately 25% of total weight lost on tirzepatide was lean mass (SURMOUNT-1 DXA substudy), and in semaglutide trials, that proportion may reach up to 40% (STEP 1 DXA subset). Resistance training and adequate protein intake can significantly reduce the lean mass deficit.
Should I get a DXA scan before starting a GLP-1 medication?
A baseline DXA scan before or soon after starting GLP-1 therapy is strongly recommended, especially for post-menopausal women, adults over 50, and anyone with known risk factors for osteoporosis. A DXA scan measures bone mineral density at the hip and lumbar spine, the same locations where the Hansen semaglutide trial documented statistically significant bone loss. Having a baseline allows the care team to monitor for changes over time and adjust the treatment plan if bone density drops into a concerning range.
What exercises should I do while on a GLP-1 to protect my bones?
Resistance training at least three times per week with compound movements is the most important intervention. Exercises like squats, deadlifts, lunges, leg presses, and overhead presses create the mechanical loading that stimulates bone formation and preserves muscle mass during weight loss. Progressive overload (gradually increasing weight or resistance over time) is key. Walking and low-impact cardio are beneficial for cardiovascular health but do not provide sufficient osteogenic stimulus to meaningfully protect bone density during rapid weight loss.
How much protein should I eat while taking Ozempic or Mounjaro?
Current guidelines from ESPEN and PROT-AGE recommend 1.2 to 1.6 grams of protein per kilogram of body weight per day for patients in catabolic states or undergoing significant weight loss. For a 180-pound (82 kg) person, that translates to approximately 98 to 131 grams of protein daily. Because GLP-1 medications suppress appetite and reduce total food intake, meeting this protein target requires deliberate planning. Prioritizing protein at every meal and considering supplementation (whey, casein, or plant-based protein) can help patients hit their daily target even when eating less overall.
