When a patient returns after anterior cruciate ligament reconstruction complaining of residual instability—that sensation of the knee “slipping” or pivoting unpredictably—standard testing often tells an incomplete story. The anterior drawer test and KT-1000 arthrometer reveal anterior translation, but they miss something equally important: rotatory laxity. Rotatory instability of the knee is not simply a complication of ACL failure. It exists on a continuum, from subtle partial rotatory laxity that compromises athletic performance to complete rotatory displacement that can undermine even well-executed ACL grafts. Understanding this continuum, and the anatomy driving it, has become central to managing the ACL patient who wants to return to pivoting sports.
The anterolateral complex (ALC) is the primary restraint to internal rotation of the knee, particularly in positions of flexion where the pivot shift occurs. This anatomic reality has driven a paradigm shift in ACL surgery: should every reconstruction include additional restraint to rotatory motion, or only those patients with documented rotatory instability? The evidence from recent research, including work from the Ochsner-Andrews Sports Medicine Institute, suggests the answer is more nuanced than one protocol fits all. This guide explores the anatomy, the consequences of missing rotatory instability, and the current evidence for anterolateral augmentation as a protective strategy.
In This Article [show]
What Is Rotatory Knee Instability?
Rotatory instability is the pathologic internal rotation (or “pivot”) of the tibia relative to the femur during weight-bearing and dynamic movement. Unlike anterior translation, which is measured in millimeters along a single axis, rotatory laxity involves multi-planar motion that creates the subjective feeling of the knee “giving way” or slipping sideways.
Dr. Burnham’s research at Ochsner, conducted in collaboration with leading international knee surgeons, has quantified rotatory instability on a clinical continuum. A landmark study by Lian, Burnham, PIVOT Study Group et al., published in the Journal of Bone and Joint Surgery in 2020, evaluated rotatory laxity in 354 patients with ACL injuries. The research identified three distinct severity levels:
- Partial rotatory laxity: 1.4 mm of tibial internal rotation displacement
- Complete rotatory laxity: 2.5 mm of displacement
- Failed ACL reconstruction with rotatory laxity: 3.3 mm or greater
This continuum matters clinically because it suggests that rotatory instability is not binary (present or absent), but rather a spectrum that may predict failure risk, symptoms, and the need for additional stabilization beyond isolated ACL reconstruction.
Why Standard Tests Miss Rotatory Laxity
Traditional ACL testing relies on the anterior drawer test and the Lachman test, both of which isolate anterior-posterior translation along a single plane. The KT-1000 arthrometer quantifies this translation numerically, giving clinicians a false sense of completeness. A patient can have a normal anterior drawer test and still have significant rotatory instability.
The problem is fundamental: these tests do not load the internal rotators. A patient lying supine with the knee flexed to 90 degrees is not in the position that provokes the pivot shift or the rotatory displacement that occurs during a cutting maneuver on the athletic field. The pivot shift test, which better captures rotatory laxity by replicating the dynamic internal rotation, is more sensitive but is subjective, difficult to perform consistently, and may be negative in patients with muscular guarding or guarding due to pain.
Modern imaging techniques, such as three-dimensional MRI and dynamic fluoroscopy, have improved visualization of rotatory displacement, but these are not routinely used in clinical practice. As a result, many patients with pathologic rotatory laxity are counseled that their ACL has been successfully reconstructed, when in fact they retain residual instability that compromises their ability to return to cutting and pivoting sports safely.
The Anterolateral Complex: Anatomy and Restraint
The anterolateral complex is a layered structure composed of the iliotibial band (ITB), the knee capsule, and deep investing layers that collectively provide the primary restraint to internal rotation of the knee, particularly in positions of 60 to 90 degrees of flexion where the pivot shift occurs.
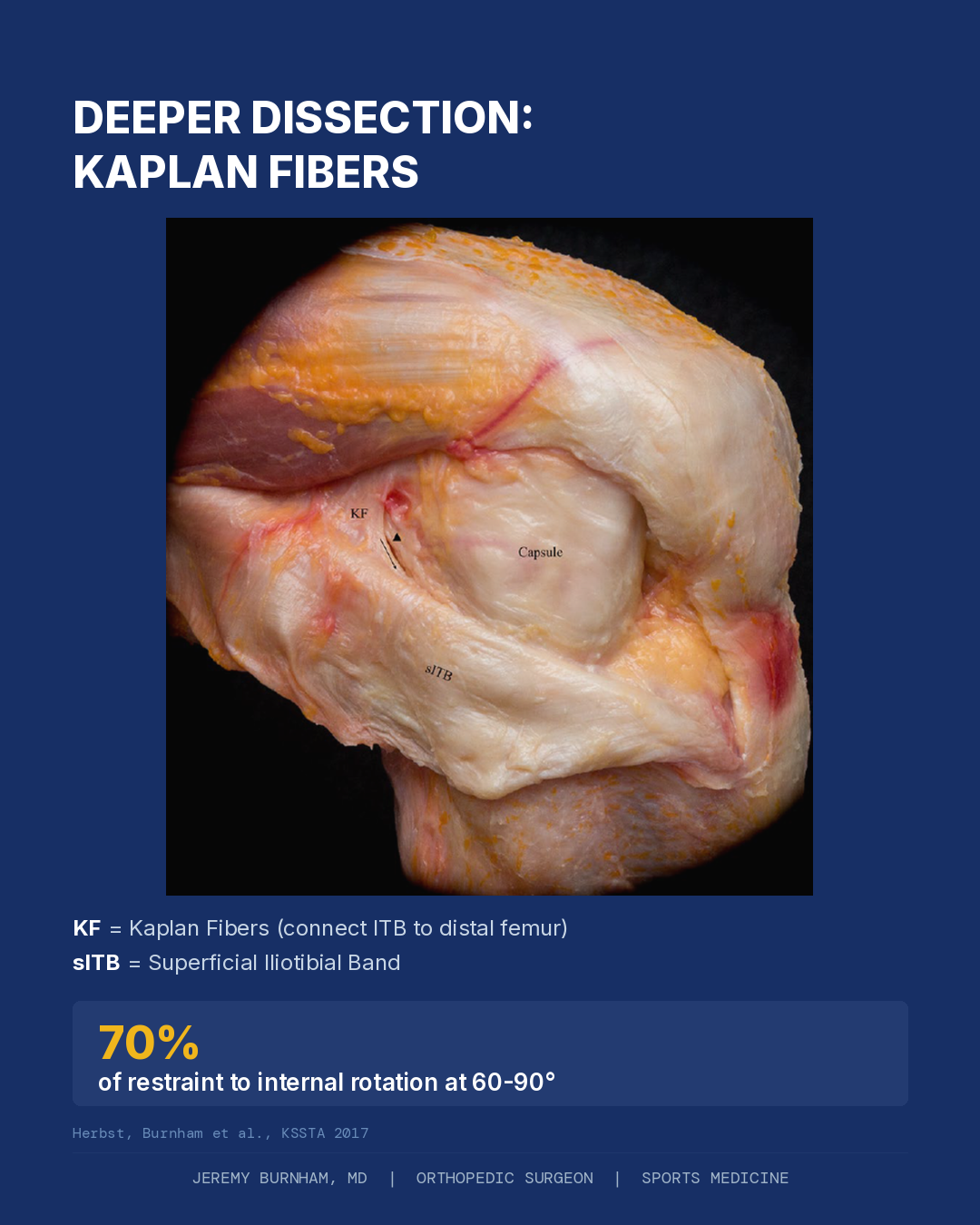
Research by Herbst, Burnham, and colleagues, published in the Orthopaedic Journal of Sports Medicine in 2017, mapped the anterolateral complex in precise anatomic detail. The superficial iliotibial band, the outermost layer, provides more than 50 percent of the restraint to internal tibial rotation on its own, in both the ACL-intact and ACL-deficient knee. The Kaplan fibers, a deeper set of fibers that anchor the ITB to the distal femoral metaphysis, add a second layer of rotational control. When these layers are considered together, the superficial and deep ITB contribute more than 70 percent of the total restraint to internal rotation at 60 to 90 degrees of flexion, the exact range where cutting, pivoting, and the pivot shift occur (Herbst, Burnham et al., OJSM 2017).
A useful way to understand this relationship: the ACL functions like a hand gripping a steering wheel near the center hub, trying to control the turn. The anterolateral complex is like a hand on the outside rim of the wheel. The hand on the outside has far more mechanical leverage to control rotation. When the anterolateral structures are damaged alongside the ACL, the hand in the center, the reconstructed ACL graft, is left trying to control rotation alone, without the leverage it needs.
The ALC’s anatomy varies between individuals. Some patients have robust, well-developed lateral capsular structures, while others have thinner or more lax tissues. This anatomic variability, combined with the severity of the original ACL injury, helps explain why some patients feel stable after ACL reconstruction while others report ongoing instability despite a technically sound graft.
Consequences of Unaddressed Rotatory Instability
The clinical consequences of untreated rotatory instability are substantial. Athletes report persistent apprehension during cutting, a sense of instability during deceleration, and fear of reinjury. Some avoid high-demand sports altogether, effectively ending competitive careers. Others experience recurrent episodes of the knee “giving out,” leading to subsequent injuries including meniscal tears and chondral damage.
Webster and Feller, in a 2016 systematic review published in the American Journal of Sports Medicine, found that patients under age 20 have an 18 percent ACL graft failure rate within a 2-year follow-up. While multiple factors contribute to graft failure, unrecognized or unaddressed rotatory instability is a significant driver, particularly in high-demand athletes returning to pivoting and cutting sports.
Compounding the problem, many patients with failed ACL grafts present with concurrent meniscal tears. In Dr. Burnham’s research cohort of 354 ACL-injured patients, 67 percent of those with failed reconstruction had meniscal pathology documented. This suggests that patients with unaddressed rotatory instability experience a cascade of secondary injuries as the unstable knee forces the meniscus to compensate for the lack of lateral rotational control.
For athletes pursuing careers in professional or elite collegiate sports, where the demand for rotational stability is maximal, the stakes are particularly high. A technically sound ACL reconstruction that fails to address rotatory instability may appear successful on paper (normal anterior drawer, favorable patient-reported outcomes at 1 year) but ultimately predispose the athlete to late-career injury or diminished performance.
Lateral Extra-Articular Tenodesis as a Solution
Lateral extra-articular tenodesis (LET), also known as anterolateral ligament augmentation, is a surgical procedure that reconstructs or reinforces the restraining structures of the ALC by securing an autologous graft (typically the iliotibial band or gracilis) to the lateral tibia at a position that controls internal rotation. When combined with anatomically placed ACL reconstruction, LET aims to restore both anterior translation and rotational stability.
International surgeon opinion on the role of LET has evolved significantly. A 2025 survey by Giusto, Burnham, and the Panther ACL Treatment Group, published in the Journal of ISAKOS, queried orthopedic surgeons worldwide on their approach to anterolateral complex augmentation. Key findings included:
- 91 percent of surveyed surgeons reported good to excellent outcomes (IKDC subjective scores, minimal pivot shift grade) when LET was added to primary ACL reconstruction
- 87 percent of patients expressed a preference for ACL plus LET over isolated ACL reconstruction when rotatory laxity was documented preoperatively
- Revision rates were lower in the combined ACL plus LET group compared to ACL-alone cases with preoperative rotatory instability (range 68 to 84 percent at 2-year follow-up)
These data suggest that in appropriately selected patients (those with preoperative rotatory instability, elite athletes, or those with failed prior reconstruction), the addition of LET provides measurable protection against recurrent instability and may improve overall functional outcomes and return-to-sport success.

Treatment Decision Framework
Not every ACL-injured patient requires LET. The decision to add anterolateral augmentation should be individualized based on several factors:
- Preoperative rotatory instability status: Documented pivot shift grade, high-grade Lachman, or imaging evidence of rotatory displacement
- Athlete’s sport and demand level: Elite athletes in pivoting and cutting sports have higher risk of failure with ACL-alone reconstruction
- Reconstruction timing and associated injuries: Chronic ACL injuries with multiple associated injuries (meniscal tears, cartilage damage) may benefit from additional stabilization
- Prior failed reconstruction: A patient with a failed ACL graft and recurrent instability is a strong candidate for combined ACL plus LET
- Patient age and longevity goals: Younger patients with high athletic aspirations warrant more aggressive rotational control strategies
For many patients with primary ACL tears and no significant rotatory laxity, an anatomically placed ACL reconstruction alone, combined with a disciplined rehabilitation program that emphasizes proprioception and neuromuscular control, provides excellent outcomes. The goal is not to perform LET on every ACL patient, but rather to identify and treat the subpopulation at highest risk of failure due to unaddressed rotatory instability.
At Ochsner-Andrews Sports Medicine Institute, our approach integrates clinical examination (pivot shift testing, dial test), imaging (MRI for ligament integrity and tibia rotation angle measurement), and athlete profile (age, sport, prior injuries) to determine who will benefit most from anterolateral augmentation. This personalized strategy has improved outcomes for athletes seeking to return not just to sports, but to the level of performance they enjoyed before injury.

The Bottom Line
Rotatory knee instability exists on a clinical continuum, from subtle partial laxity that affects athletic performance to complete rotatory displacement that undermines surgical reconstruction. The anterolateral complex is the primary restraint to this motion, and standard anterior translation tests often fail to detect pathologic internal rotation. In patients with documented rotatory instability, particularly elite athletes or those with failed prior reconstruction, the addition of lateral extra-articular tenodesis to anatomic ACL reconstruction improves outcomes and reduces revision rates. The key is not to pursue one protocol for all patients, but to identify the subset at highest risk and tailor surgical strategy accordingly. For athletes seeking to return not just to sport, but to perform at their highest level, addressing rotatory instability is essential.
“Rotatory instability is one of the most underrecognized causes of poor outcomes after ACL reconstruction. When we identify it early, and address it with appropriate surgical strategy, our athletes get back to the sports they love with confidence. This is what precision orthopedic surgery is about.” — Dr. Jeremy Burnham, Sports Medicine Specialist, Ochsner-Andrews Sports Medicine Institute

References
- Lian J, Diermeier T, Meghpara M, PIVOT Study Group, et al. “Rotatory Laxity of the Knee in Anterior Cruciate Ligament Injury: A Continuum of Instability.” Journal of Bone and Joint Surgery American, 2020. PMID: 32379120
- Herbst, E., Burnham, J. M., et al. “The Anterolateral Complex of the Knee: A Review of Anatomy.” Orthopaedic Journal of Sports Medicine, 2017. PMID: 28451619
- Webster, K. E., & Feller, J. A. “Exploring the High Reinjury Rate in Australian Rules Football After Anterior Cruciate Ligament Reconstruction: A Case-Control Study.” American Journal of Sports Medicine, 2016. PMID: 27390346
- Giusto JD, Konstantinou E, Rabuck SJ, Panther ACL Treatment Group, et al. “Anterolateral Ligament Augmentation in Anterior Cruciate Ligament Reconstruction: International Surgeon Survey on Indications and Outcomes.” Journal of ISAKOS, 2025. DOI: 10.1016/j.jisako.2025.01.001
- Burnham, J. M. “The Anterolateral Complex in Acute and Chronic Anterior Cruciate Ligament Injuries: Review of Anatomy and Clinical Significance.” Journal of Clinical Orthopedics, 2016. PubMed
- Musahl, V., Burnham, J. M., et al. “The Role of the Anterolateral Structures and the Anterior Cruciate Ligament in Controlling Knee Laxity.” Knee Surgery, Sports Traumatology, Arthroscopy, 2017. PubMed
For a comprehensive overview of ACL reconstruction and surgical options at Ochsner-Andrews, or to discuss treatment for complex knee injuries and sports medicine concerns, Dr. Burnham invites you to schedule a consultation. Understanding your specific injury pattern, combined with your athletic goals, allows for a personalized surgical strategy that addresses not just anterior stability, but the full spectrum of knee laxity.
Frequently Asked Questions
The pivot shift test is a dynamic examination where the examiner applies a valgus and internal rotation force to the knee, reproducing the subluxation and reduction that occurs in rotatory instability. Unlike the anterior drawer test, which isolates anteroposterior translation, the pivot shift loads the rotatory restraints and replicates the instability experienced during cutting and pivoting sports. While more sensitive for rotatory laxity than standard tests, the pivot shift can be difficult to elicit if the patient has muscular guarding or pain. A positive pivot shift, combined with clinical history, strongly suggests the need for careful preoperative assessment and potential consideration of combined ACL plus lateral extra-articular tenodesis reconstruction.
Yes. The KT-1000 arthrometer specifically measures anteroposterior translation and is not designed to detect internal or external rotation. A patient can have normal anterior laxity (within normal limits on KT-1000) and still have pathologic rotatory instability. This is why clinical examination, including the pivot shift test, and dynamic imaging, if available, are essential complements to quantitative translation testing. Many athletes with failed or functionally inadequate ACL reconstructions have normal anterior translation but persistent rotatory laxity.
Not every ACL reconstruction requires LET. Patients with primary ACL injuries, no significant preoperative rotatory instability, and lower athletic demands often achieve excellent outcomes with anatomically placed ACL reconstruction alone. However, patients with documented rotatory instability, elite-level athletes in cutting and pivoting sports, those with failed prior reconstruction, or those with chronic ACL injuries and multiple associated injuries are strong candidates for combined ACL plus LET. The decision should be individualized based on injury severity, athlete profile, and functional goals.
The most commonly used grafts for LET are autologous tissues, either the iliotibial band (ITB) or the gracilis tendon. The ITB provides excellent length and strength, while the gracilis offers a smaller footprint and reduced morbidity at the harvest site. Both have shown good outcomes when secured to the lateral tibia in a position that controls internal rotation during 60 to 90 degrees of knee flexion. Graft choice depends on surgeon preference, tissue quality, and concurrent reconstructions being performed.
Recovery from combined ACL plus LET is typically 4 to 6 months longer than isolated ACL reconstruction, with full return to pivoting and cutting sports expected around 12 months. The added time accounts for both the ACL graft maturation and the healing of the lateral extra-articular augmentation. Rehabilitation emphasis on proprioception, neuromuscular control, and sport-specific conditioning remains essential to restore confidence and function. Athletes should be counseled that patience and adherence to the rehabilitation protocol are critical for optimal outcomes.
